Jaclyn K. Schwartz, MS, OTR/L
Roger O. Smith, PhD, OT, FAOTA, RESNA Fellow
Introduction
In the past year, physicians prescribed over two-billion medications to patients seeking medical services (Centers for Disease Control and Prevention, 2013). While physicians hope their patients will take their medications as prescribed, more than 50% of patients simply do not, demonstrating impairments in medication adherence, or the “degree of correspondence between the patient’s actual dosing history and the prescribed regimen” (Barber, Parsons, Clifford, Darracott, & Horne, 2004; Schaffer & Yoon, 2001). Good medication adherence is essential to receiving the health benefits associated with the medication. Shepard and colleagues (1997) found that patients with cardiac conditions must take at least 75% of their medication to receive benefits, otherwise they are no better off than the placebo group. Additionally, poor adherence to medication regimens can cause hospitalization, admission to assisted living facilities for older adults, increased health care spending, adverse events (such as heart attack or stroke), and even death (Kripalani, Yao, & Haynes, 2007; Krueger, Berger, & Felkey, 2005; Schaffer & Yoon, 2001).
Given the large impact of medication non-adherence on patients, providers, and payors, medication management has been the topic of great research in recent decades. Unfortunately, most research has been conducted by large research-based multidisciplinary teams who have been guided by the medical model, with research from allied health professionals lacking (Haynes R.B., Ackloo E., Sahota N., McDonald H.P., & X., 2008).
The lack of research by allied health or rehabilitation professionals, poses many questions about the research findings. Medication management is a complex and dynamic activity that involves not only the persons’ impairments, but the social and physical environment, and the choice of and training with the assistive technology devices. Medication management often includes the use of low-tech pill boxes and reminder systems, but the array of devices is much more substantial. Pill splitters, activity tracking systems, and automated pill dispenser systems are examples of the rapidly growing availability of assistive technologies. The lack of rehabilitation professionals present in research when juxtaposed to multidimensionality of the needed evaluation and intervention demonstrates a disconnect between research and practice.
The purpose of this critical review is to decrease the disconnect by reviewing existing literature in medication management and applying it to assistive technology practice models that portray the complexity and acknowledge the covariates of assistive technology intervention (Cook & Hussey, 1995; Smith, 2005). Specifically, this review examines the constructs in the Cook & Hussey model of Human Activity Assistive Technology (HAAT). In this article, we will review current research in medication management evaluation and intervention with this assistive technology frame of reference. Then we will make recommendations to practitioners and researchers in this field of study.
Methods
We conducted comprehensive literature searches for review articles published between 2003 and 2013. The Medline and CINAHL databases were searched for reviews of assessments. The Cochrane database was searched for intervention reviews. The following key word were used: patient compliance, adherence, medication, and outcome and process assessment. To be selected for this paper, the authors had to review two or more specific assessments or interventions for medication management.
Data Analysis
Once the literature review was complete articles were gathered, the manuscripts were loaded in to Dedoose, a cross-platform application for quantitative analysis. Evaluations and interventions were coded for their use of assistive technology and other major components of the HAAT model. If researchers were unable to code an evaluation or intervention, the original article was retrieved and used to fill in any gaps in information.
Results
Intervention
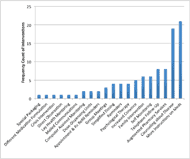
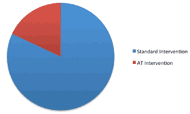
One Cochrane Review was found on the topic of medication management (Haynes R.B. et al., 2008). Haynes and Colleagues detailed 78 randomized controlled trials testing 100 different interventions divided into 20 categories. Researchers tested a variety of interventions, with no one intervention demonstrating enough success to be declared a gold-standard. Education about a person’s medication or health condition was the most used intervention. Assistive technology was found across studies and was directly named in 18% of interventions. Some assistive technology interventions included reminders delivered via a smartphone or computer, special packaging (e.g. blister packs), and even dose-dispensing robots.
The use of assistive technology based interventions also may be under reported. For example Schroeder, Fahey, Hollinghurst, & Peters (2005) used a nurse led educational intervention. The protocol encouraged the nurse leading the educational experience to “find individual solutions to patients’ problems” (p. 145). The authors, however, did not elaborate on types of individual solutions or if assistive technology was involved. The neglect of considering assistive technology as a factor, even when it is a key component of an intervention, is not uncommon (Rust & Smith, 2005)..
Finally, because all studies reviewed were part of randomized control trials, the researchers implemented protocols that may detract from clients existing routine including the use assistive technology. For example, seven studies used a Medication Event Monitoring System (MEMS) to measure outcomes. MEMSs are electronic pill bottle caps that measure when the bottle was opened, indicating that a person took their medication. While MEMS caps improve the reliability of medication adherence numbers, the caps also require the participant to keep their medication in the bottle, thereby preventing participants from using adaptive strategies such as a pill box.
Assessment
We found two articles that identified 18 assessments that measure medication management abilities (Elliott & Marriott, 2009; Farris & Phillips, 2008). Eleven (61%) of those assessments were redundant between the two articles, indicating good saturation.
The HAAT model states that assistive technology practitioners should consider the human, the activity, assistive technology, and the context during evaluation and intervention. The assessments in medication management were limited in scope and often tested the persons cognitive and sensory skills by having the client open medication bottles, manipulate the pills, and sort and/schedule pills into a pill box (Elliott & Marriott, 2010). Most assessments did not evaluate the context in terms of medication storage or pharmacy access, and no assessments investigated current habits, roles, routines.
Not only did the assessments fail to measure the activity and the context, but they also fail to measure assistive technology. Many of the assessments require a client to fill a pill box, without regard for what the person already has in their home. Furthermore, the pill boxes used in the assessment vary in features. For example Figures 3 and 4 demonstrate the pill boxes used in the Self-Medication Task and the Hopkins Medical Schedule. The pill box in the Self-Medication Task is more complex due to the many smaller compartments making the task more physically and cognitively challenging. Additionally, each assessment generally uses only one form of pill box, thereby hindering a clinicians ability to understand which pill box might be the best fit to enhance medication compliance.
Finally, despite the presence 18 assessments available in the literature that evaluate capacity for medication management, none of these assessments were used by the interventionist in the Cochrane Review article. Instead, the interventionist used generic or symptom specific measures such as the SF-36, HbA1c (blood glucose levels), or the Minnesota Living with Heart Failure Questionnaire. While these measures generally have better reliability and validity for research, they do not investigate use of assistive technology at baseline or at the completion of the study.
Discussion
Assistive technology is widely used in medication management interventions. While few researchers included in the Cochrane review verbalized assistive technology components, seemingly many interventions have components that went unrecognized. Perhaps one reason is that the researchers failed to recognize assistive technology use in their evaluation plan, leaving the impact of assistive technology on medication compliance unclear. Additionally, the rigorous protocols utilized by the researchers in the Cochrane review decreased the subjects ability to use assistive technology (if they did so before) which could have artificially decreased the subject’s performance in medication adherence.
The assessments available for medication management also demonstrated several challenges for assistive technology practitioners. The content of the assessments is not holistic and lacks the vital components required by the HAAT model. Specifically, no assessments inquired about current assistive technology use, some assessments assumed the use of a pill box. Sanders & Van Oss (2013) found that only 65% of their sample of older adults used a pill box at home, indicating that the use of a pill box is not a safe assumption. Furthermore, there was great variation on the pill boxes utilized in the assessment presenting the client with different challenges.
Perhaps because of the many issues demonstrated by the assessment literature, interventionist choose to use more popular and standardized measures in their randomized control trials, indicating a gap between evaluation and intervention. To measure progress some assessments need utility at the beginning and the end of intervention.
Conclusion
Poor medication adherence is a major public health issue that can cause hospitalization, poor health outcomes, and even death. Medication adherence is a complex problem that is affected by activity, assistive technology use, context, and human factors. Unfortunately, both the assessments and the interventions over emphasize impairment and training while neglecting the activity, the assistive technology, and the context. Assistive technology professionals, given their unique perspective that accounts for the assistive technology, context, and activity factors have potential to increase the standards of care in medication management. Unfortunately, the tools and research are not available to meet the needs of practitioners. More research is needed that focus on the role of assistive technology and context in medication management.
References
Barber, N., Parsons, J., Clifford, S., Darracott, R., & Horne, R. (2004). Patients’ problems with new medication for chronic conditions. Quality and Safety in Health Care, 13(3), 172-175.
Centers for Disease Control and Prevention. (2013). Therapeutic Drug Use. Retrieved January 6, 2014, from http://www.cdc.gov
Cook, A. M., & Hussey, S. M. (1995). Assistive technologies: Principles and practice. St. Louis, MO: Mosby. ,
Elliott, R. A., & Marriott, J. L. (2009). Standardised assessment of patients' capacity to manage medications: a systematic review of published instruments. BMC geriatrics, 9(1), 27.
Elliott, R. A., & Marriott, J. L. (2010). Review of instruments used in clinical practice to assess patients’ ability to manage medications. J Pharm Pract Res, 40, 36-42.
Farris, K., & Phillips, B. (2008). Instruments assessing capacity to manage medications. The Annals of pharmacotherapy, 42(7), 1026.
Haynes R.B., Ackloo E., Sahota N., McDonald H.P., & X., Y. (2008). Interventions for enhancing medication adherence. Cochrane Database of Systematic Reviews.
Kripalani, S., Yao, X., & Haynes, R. B. (2007). Interventions to enhance medication adherence in chronic medical conditions: a systematic review. Archives of internal medicine, 167(6), 540.
Krueger, K., Berger, B., & Felkey, B. (2005). Medication adherence and persistence: A comprehensive review. Advances in Therapy, 22(4), 313-356.
Rust, K. L. & Smith, R. O. (2005). Assistive technology in the measurement of rehabilitation and health outcomes: A review and analysis of instruments. American Journal of Physical Medicine and Rehabilitation, 84 (10), 780-793.
Sanders, M. J., & Van Oss, T. (2013). Using Daily Routines to Promote Medication Adherence in Older Adults. The American Journal of Occupational Therapy, 67(1), 91-99.
Schaffer, S. D., & Yoon, S. L. (2001). Evidence-based methods to enhance medication adherence. Nurse Practitioner, 26(12), 44-44, 50, 52.
Schroeder, K., Fahey, T., Hollinghurst, S., & Peters, T. J. (2005). Nurse-led adherence support in hypertension: a randomized controlled trial. Family Practice, 22(2), 144-151.
Shepherd, J., Cobbe, S., Lorimer, A., McKillop, J., Ford, I., Packard, C., Lever, A. (1997). Compliance and adverse event withdrawal: their impact on the West of Scotland Coronary Prevention Study. European Heart Journal, 18(11), 1718-1724.
Smith, R.O., IMPACT 2 Model, (1995), Retrieved January 13th, 2014 from http://www.r2d2.uwm
Audio Version PDF Version