Leighanne M. Davis1, Kevin Caves1,2
1Duke University Head and Neck Surgery & Communication Sciences, 2Duke University Department of Surgery, Medicine and Biomedical Engineering
INTRODUCTION
Information communication technology (ICT), is a term used to describe technologies designed around software, networking, telecommunications, Internet, programming, and information systems.[1] These emerging technologies have been a focus area for healthcare and related industries because of their ability to communicate vital / helpful information to clinicians and users, provide timely interventions, and improve overall quality of life over various ages and disease states. Although ICT has gained momentum within healthcare, the older adult population is still an underrepresented group in terms of technological advancement. There are constraints and barriers to enabling new technology with the older adult population, but research supports the claim that older adults are adopting new technology.[2] In fact, a 2014 Pew study found that 59% of older adults use the Internet, 78% have a cell phone, 62% have a computer, 22% a smartphone, and 25% a tablet. While the smartphone and tablet percentages are about 20-30% lower than all adults [3], cellular, computer, and online use point to a positive trend of technology adoption amongst older adults. Considering the U.S. Census Bureau estimates that by 2050 about 1 in 5.2 Americans will be above the age of 65 [4], it is important for additional ICT development within this population.
APPROACH
Three examples of technologies developed for older adults are described. These technologies focus on easy to use interfaces, low-cost designs, and accurate measurements / reporting. While the intended users of these products are older adults, the flexibility of the designs can also be used to benefit other populations.
Gait Box
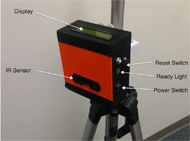
Overall Operation & Features
The Gait Box works by use of a low-cost IR sensor, microcontroller, and 3D printed parts. The microcontroller determines the velocity of a person via distance data from the IR-proximity sensor and time data from the microcontroller’s internal clock. An LED indicates to the user when to walk and when data is being captured. Walking speed is displayed in an easy to read format on an LCD screen (Figure 1). The device can be programmed to measure gait speed at different distances up to 6 meters. This device is easy to move because of its lightweight design and can be mounted on an IV pole, tripod, or wall for measurements.
One Thing Straight
Individuals with Parkinson’s disease (PD) often have postural instability.[8] This instability can be accompanied by a decrease in postural awareness associated with not recognizing a flex or bent posture, often perceiving the bent posture as being straight.[9] Posture changes can be dangerous and often lead to an increased number of falls and potential injury.[8] With visual reminders, such as observing posture in a mirror or audio reminders from other individuals, people with PD can often momentarily correct their posture.[10] The phone application, One Thing Straight aims to reduce the incidence of fall or injury by automatically measuring postural changes and notifying the user.
Overall Operation & Features
One Thing Straight is an app plus microcontroller based sensor programmed to recognize postural movements. The microcontroller used is the LightBlue Bean by PunchThrough Design. This microcontroller has wireless programming capabilities, an accelerometer, thermometer, RGB LED, is Arduino-compatible, and has built in Bluetooth Low Energy (BLE). The Bean sends accelerometer data to the iOS or Android phone application via a company supplied SDK, where the phone application determines postural movements. When an incorrect posture is determined, the user is notified by a discrete tone or vibration from the phone application indicating they need to correct their posture. These times of incorrect posture can be recorded and used by clinicians or the user to track postural instability over time. The system can be calibrated daily for accurate measurements and can be used while sitting or standing. The Bean is positioned inside of the user’s shirt collar as to not be noticeable or disturb the user.
Safe@Night
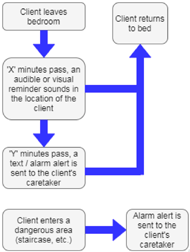
Overall Operation & Features
Safe@Night is a system of sensors, microcontrollers, and communication protocols designed to monitor users throughout the night and provide auditory or visual cues to return to bed. The system is centered around stand-alone devices that communicate with each other to track the user. If it has been determined that the user has been out of bed for ‘X’ minutes, a cue is played indicating to the user to return to bed. If the user returns to bed the system resets and waits for the next movement out of bed. Otherwise, the system alerts the user’s caregivers via wireless communication (Figure 2). A log of movements throughout the night is recorded for the caregiver or clinicians.
RESULTS
Gait Box
A validation study between the Gait Box, a stop watch and technician, and the Sprint System from Brower Timing is underway. This study will take place on clinically appropriate individuals at Duke University Health System (DUHS) in Durham, NC. At the completion of validation testing, additional studies will be conducted in outpatient geriatric clinics at DUHS to test clinician response and acceptance. Informal testing shows positive results.
One Thing Straight
The PD posture system has been deployed to one user for feedback and active daily use. This user found the device comfortable and concealable. The user appreciated the discrete notification system and noted that it allowed for the device to blend into the physical environment. After testing, the user completed a short survey, indicating intended long-term use. Specifically, the user stated, “It is working perfectly – hardly know it is in the T-shirt! Even the presence of the device reminds me to correct my position.”
Safe@Night
Development is still underway for the Safe@Night system and therefore testing has not been completed. Once complete, testing will take place on a clinically relevant population.
DISCUSSION
Gait Box
Currently designed to be implemented within a hospital or clinical setting to measure a patient’s walking speed, future iterations of the device will allow for an at home component that will passively monitor the user’s walking speed. It is believed that this will give clinicians valuable longitudinal feedback in-between visits. This feedback can potentially help determine the need for a clinical visit in-between regularly scheduled visits if walking speed is significantly reduced or can help provide insights into progress post evaluation / surgery.
One Thing Straight
The app has been designed to understand how postural angle changes between sitting and standing so that it can properly notify the user during these instances. Special considerations have also been made to distinguish between a user reaching for an object or actual postural changes. This is accomplished by the phone app looking for a sustained position of at least 20 seconds. If the user is in an incorrect posture for less than 20 seconds, it is determined that they were reaching for an object or recognized their posture and were able to take appropriate action independently. A bent posture of 20 seconds or more indicates that the user is in an incorrect posture.
Like other wearable technology, the hardware component of One Thing Straight has reduced battery capacity due to continuous streaming of data to the cellular phone. Although the device can last at least 8 hours for standard wear, increasing the battery life would be a big benefit for wearers. Current solutions involve custom code on the microcontroller itself to decrease the sampling rate. In the future, handling battery consumption would ideally take place within the phone application as to reduce the need for additional programming and potential data transfer errors.
Safe@Night
Although Safe@Night is still in its infancy as far as development and project completion, the overall goal to reduce the incidence of dangerous nighttime wandering is being met with each prototype design. Special considerations have been made for the modular aspect of this system because not all user’s live in similar settings: some users may be in an assistive living facility, some with family, and even some user’s may be relatively independent. This modular aspect also allows for the system to be used in different size homes and facilities, such as a small apartment to an assistive living facility.
CONCLUSION
All three projects fulfill the basic need for ICT development for older adults. These projects focus on utilizing low-cost, readily available, and easy to use components. With an aging U.S. population, increased technology development is very important for older adults to help them age well and live independently.
REFERENCES
[1] University of Kentucky College of Communication and Information (2017, Oct. 18). Information Communication Technology. Retrieved Oct. 18, 2017, from https://ci.uky.edu/sis/ict.
[2] Mitzner, Tracy L., Boron, Julie B., et al. (2012, Nov.). “Older adults talk technology: Technology usage and attitudes.” Computers in Human Behavior, 26(6): 1710-1721.
[3] Zickuhr, Kathryn. (2014, April 29). “Older adults and technology.” Pew Research Center presentation JASA – New York, NY. Retrieved Oct. 20, 2017, from http://www.pewinternet.org/files/2014/07/kzickuhr-Seniors-and-Tech-JASA.pdf.
[4] Ortman, Jennifer M., Velkoff, Victoria A. (2014, May). “An Aging Nation: The Older Population in the United States.” Population Estimages and Projections: P25-1140.
[5] Guralnik, JM, L Ferrucci, et al. (2000). “Lower extremity function and subsequent disability: consistency across studies, predictive models, and value of gait speed alone compared with the short physical performance battery.” J Gerontol: MS 55A(4): M221-M231.
[6] Lusardi, Michelle M. (2012). “Is Walking Speed a Vital Sign? Absolutely.” Topics in geriatric rehabilitation 28(2): 67-76.
[7] Studenski S, S Perera, et al. (2011). “Gait speed and survival in older adults.” JAMA 305(1): 50-58 10.1001/jama.2010.1923.
[8] Nonnekes, J., Goselink, R., Weerdesteyn, V., Bloem, B.R. (2015). “The retropulsion test: a good evaluation of postural instability in Parkinson’s disease?” Journal of Parkinson’s Disease, 5(1): 43-7. doi: 10.3233/JPD-140514.
[9] Monique L. Giroux. Northwest Parkinson’s Foundation (2014, March 21). PD Community Blog: Parkinson’s Posture. Retrieved Oct. 18, 2017, from https://nwpf.org/stay-informed/blog/2014/03/parkinsons-posture/.
[10] National Parkinson Foundation. Tip Sheet: Posture and Parkinson’s. Retrieved Oct. 18, 2017, from www.parkinson.org/pd-library/fact-sheets/posture-and-parkinson-s.
[11] Anderson, C., Law, J. Kiely, Daniels, A., Rice, C., Mandell, D.S, Hagopian, L., Law, P.A. (2012). “Occurrence and Family Impact of Elopement in Children with Autism Spectrum Disorders.” Pediatrics, 130(5). Doi:10.1542/peds.2012-0762d.
[12] Hughes Julian C, Louw Stephen J (2002). “Electronic tagging of people with dementia who wander.” BMJ 325(7369): 847-848.
ACKNOWLEDGEMENTS
This work is supported by the Rehabilitation Engineering Research Center for Information and Communications Technology Access (LiveWell RERC). The LiveWell RERC is funded by a 5-year grant from the National Institute of Disability, Independent living and Rehabilitation Research (NIDILRR) in the U.S. Department of Health and Human Services (grant number 90RE5023). Analysis and opinions expressed here are those of the authors and do not reflect those of the U.S. Department of Health and Human Services or NIDILRR. This work was also sponsored by the National Institute of Aging, Claude D. Pepper Older Americans Independence Center at Duke University.
We would like to thank the following people / groups for their support: One Thing Straight: Duke Institute for Health Innovation (DIHI), Manvi Gupta, BME undergraduate students; Katherine Lee, Zoe Roecker, and Alex Kanaris. Gait Box: Jon Usher, Laura Previll MD, Ashley Kinsey. Safe@Night: Raiyan Sobhan.