Margaret E. French1, Alyssa J. Schnorenberg1,2, Briana N. Magruder1, Justin M. Riebe1, Ryan R. Inawat3, Dana H. Washburn1, Dara J. Mickschl3, Steven I. Grindel3, Brooke A. Slavens1
1University of Wisconsin-Milwaukee; 2Marquette University; 3Medical College of Wisconsin
INTRODUCTION
Approximately one quarter of U.S. adults will have a rotator cuff (RC) tear in their lifetime, and about 300,000 RC repair surgeries are performed annually [1]. The supraspinatus is the most commonly torn rotator cuff muscle requiring surgical repair [2]. RC tears can impede physical function, such as one's ability to perform activities of daily living (ADLs), and maintain functional independence [3,4]. The American Occupational Therapy Association defines ADLs as the tasks of taking care of one’s own body [5]. The goal of surgical repair is to decrease pain, increase range of motion (ROM), and allow return to the workforce [6]. Although patients may be able to perform ADLs independently before surgery, they may be using altered kinematics due to injury and pain. While studies have compared post-operative thoracohumeral (humerus relative to thorax) joint kinematics of various populations, there is no known research assessing upper extremity (UE) joint kinematics of ADLs pre- and post-operatively, which may provide insight on the rehabilitation process. [7,8]. The purpose of this study is to compare glenohumeral (GH) joint kinematics of three ADLs and shoulder function before and after supraspinatus repair surgery. It is hypothesized that GH joint kinematics and functional shoulder outcomes will be significantly different following rotator cuff surgery.
METHODS
Subjects
Six (6) adult subjects (63.5 ± 7.1 years) with a full-thickness, supraspinatus RC tear participated in this study (Table 1). Subjects who had a previous shoulder surgery, currently have systemic inflammatory arthritis, or shoulder pathology in both shoulders were excluded. This study was approved by the University of Wisconsin-Milwaukee (UWM) Institutional Review Board; written informed consent was obtained from each participant.
| Subject | Gender | Surgical Arm | Dominant Arm | Tear Thickness | Tear Size (cm) | Age (years) | Pre session to Surgery (days) | Surgery to Post session (days) |
|---|---|---|---|---|---|---|---|---|
| 1 | F | R | R | Full | 1.25 | 59 | 34 | 78 |
| 2 | M | L | R | Full | 1.50 | 75 | 2 | 85 |
| 3 | F | L | R | Full | 1.00 | 55 | 19 | 71 |
| 4 | M | R | R | Full | 1.00 | 66 | 4 | 79 |
| 5 | F | R | R/L | Full | 2.50 | 66 | 9 | 76 |
| 6 | M | R | R | Full | 4.00 | 60 | 5 | 80 |
| Average ± SD | 1.9 ± 1.2 | 63.5 ± 7.1 | 12.2 ± 12.2 | 78.2 ± 4.6 |
Data collection

Data processing
All data was processed using Vicon Nexus Software to label marker trajectories, fill gaps, and filter the data (Figure 1). A custom inverse dynamics model [12] was used to calculate the three-dimensional (3-D) upper extremity joint kinematics. The 3-D GH joint angles were calculated as the motions of the humerus relative to the scapula. Peak angles and ranges of motion (ROM) were determined for each trial, and the group means and standard deviations were computed for each task. The Wilcoxon signed-ranks test, a nonparametric statistical procedure, compared pre-operative to post-operative sessions (p < 0.05) via IBM SPSS Statistics (IBM, Armonk, NY).
RESULTS
Glenohumeral joint kinematics
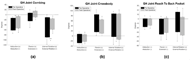
Shoulder functional outcomes
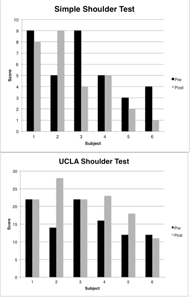
While there was no significant difference between the group average SST scores pre (5.8 ± 2.6) to post (4.8 ± 3.2, p=0.343). Although there were no significant differences in the SST scores within the group, subject 2’s score did increase to 9 post- operatively (Figure 3). Although there was no significant difference between the group average UCLA scores pre (16.3 ± 4.6) to post (20.7 ± 5.7, p=0.144), there was substantial individual variability. Three subjects’ scores increased (subjects 2, 4 and 5), two stayed the same (subjects 1 and 3) and 1 decreased (subject 6) (Figure 3). Additionally, for the UCLA question regarding satisfaction with the affected limb, five subjects reported an increase post- operatively. Active forward flexion on the UCLA scores averaged 129.2° at 9-12 weeks post-operatively.
DISCUSSION
We examined ADLs to evaluate functional performance. We found a significant difference in GH joint external rotation ROM and a decreased maximum abduction angle during the combing task. When combing the hair, less external rotation, while abducted, increases the subacromial space, thereby reducing the risk of shoulder impingement. Although we found differences in external rotation ROM, a recent study found differences in internal rotation during the combing task [7]. Patients may still retain independence with functional tasks pre and post-operatively even if they do not achieve what is considered full shoulder ROM. A study conducted on healthy females found the minimum angles required to perform the combing hair task were 73 degrees of GH scaption, 38 degrees of GH external rotation, and 112 degrees of elbow flexion [13]. Although obtaining full motion is a reasonable goal by therapists for shoulder treatment, less ROM may be sufficient to perform functional tasks and still be independent. Significant differences were found in the average maximum abduction angle (decrease) and maximum external rotation angle (increase) for the combing task. Subjects’ ROM was the same, but they may be reallocating ROM amongst different planes to still complete the task. After surgery, the mechanics of the joint may change during the recovery process when structures have been restored to their original function.
We found no significant differences in the SST score at 9-12 weeks, which is similar to other findings of subjects not improving at this point in time [14,15]. Healthy subjects scored within the range of 9 to 12, so subject 2’s post- operative score of 9 indicates they reached healthy shoulder function range [16]. Although it depends on the physician and clinic, most current rehabilitation protocols suggest patients have full active ROM by post-operative week 12. Mean UCLA item scores of active forward flexion (129.2°) demonstrates patients are close to recovering almost full range of motion of the allowed 180 degrees (71.8%). Pre-operative knowledge could help therapists identify a change in intervention or rehabilitation protocols to benefit those who are not progressing as well as other patients. Other factors to consider in future analyses are age, duration of symptoms, tear size, and pre-post window time.
CONCLUSION
We were able to successfully compare GH joint kinematics during three ADLs and shoulder assessments before and after a RC repair surgery. Although patients may be able to perform ADLs independently before surgery, they may be using altered kinematics and compensation strategies due to injury and pain. A comparison of the pre-operative
Figure 3. Individual subjects’ pre-operative (black) and post-operative (gray) scores of the SST and UCLA functional shoulder assessments.
to post-operative performance may influence appropriate rehabilitation after surgery. Research is underway to investigate shoulder motion, pain, and function in a larger population with additional ADLs. Ultimately this work may aid occupational therapists in ADL interventions to improve rehabilitation outcomes and increase independence.
REFERENCES
[1] Crawford M. Does age affect surgically repaired rotator cuffs? OREF-funded study looks at pathophysiology of tendon-to-bone healing in older patients. AAOS Now. 2014: 34.
[2] Opsha O, Malik A, Baltazar R, Primakov D, Beltran S, Miller TT, et al. MRI of the rotator cuff and internal derangement. Euro J Radiol. 2008 68(1):36-56.
[3] Lin JC, Weintraub N, Aragaki DR. Nonsurgical treatment for rotator cuff injury in the elderly. J Am Med Dir Assoc. 2008 9(9):626-632.
[4] Walker-Bone K, Palmer KT, Reading I, Coggon D, Cooper C. Prevalence and impact of musculoskeletal disorders of the upper limb in the general population. Arthritis Rheumatol. 2004 51:642–651.
[5] American Occupational Therapy Association. Occupational therapy practice framework: Domain and process (3rd ed.). Am J Occ Ther. 2014 68 (Suppl.1):S1-S48.
[6] Day A, Taylor NF, Green RA. The stabilizing role of the rotator cuff at the shoulder-responses to external perturbations. J Clin Biomech. 2012 27(6):551-556.
[7] Fritz JM, Inawat RR, Slaven BA, McGuir JR, Ziegler DW, Tarima SS, et al. Assessment of kinematics and electromyography following arthroscopic single-tendon rotator cuff repair. PM R. 2017 9(5):464-476.
[8] Vidt ME, Santago II AC, Marsh AP, Hegedus EJ, Tuohy CJ, Poehling G, et al. (2016). The effects of a rotator cuff tear on activities of daily living in older adults: a kinematic study. J Biomech. 2016 49(4): 611- 617
[9] Godfrey J, Hamman R, Lowenstein S, Briggs K, Kocher M. Reliability, validity, and responsiveness of the simple shoulder test: Psychometric properties by age and injury type. J Shoulder Elbow Surg. 2007 16(3): 260-267.
[10] Smith MV, Calfee RP, Baumgarten KM, Brophy RH, Wright RW. Upper extremity-specific measures of disability and outcomes in orthopaedic surgery. J Bone Joint Surg Am. 2012 94(3):277-285.
[11] Kirkley A, Griffin S, Dainty K. Scoring systems for the functional assessment of the shoulder. Arthroscopy. 2003 19(10):1109-1120.
[12] Schnorenberg AJ, Slavens BA, Wang M, Vogel LC, Smith PA, Harris GF. Biomechanical model for evaluation of pediatric upper extremity joint dynamics during wheelchair mobility. J Biomech. 2014 47:269-276.
[13] Magermans DJ, Chadwick EKJ, Veeger HEJ, Van Der Helm FCT. Requirements for upper extremity motions during activities of daily living. J Clin Biomech. 2005 20(6): 591–599.
[14] Kim YS, Chung SW, Kim JY, Ok JH, Park I, Oh JH. Is early passive motion exercise necessary after arthroscopic rotator cuff repair? Am J Sports Med. 2012 40(4): 815–821.
[15] Austin L, Pepe M, Tucker B, Ong A, Nugent R, Eck B, Tjoumakaris F. Sleep Disturbance Associated With Rotator Cuff Tear: Correction With Arthroscopic Rotator Cuff Repair. Am J Sports Med. 2015 43(6):1455–1459.
[16] Clarke MG, Dewing CB, Schroder DT, Solomon DJ, Provencher MT. Normal shoulder outcome score values in the young, active adult. J Shoulder Elbow Surg. 2009 18: 424-428.
ACKNOWLEDGEMENT
This study was supported under grants from the University of Wisconsin-Milwaukee College of Health Sciences and the Medical College of Wisconsin Department of Orthopaedic Surgery. We would like to thank Andrew Barnett for assisting with subject recruitment.