Emily A. Kringle, MOT, OTR/L; I Made Agus Setiawan, MSc; Bambang Parmanto, PhD; Elizabeth R. Skidmore, PhD, OTR/L
School of Health and Rehabilitation Sciences, University of PittsburghAbstract
The iADAPTS mobile health system was developed to support the delivery of a meta-cognitive rehabilitation intervention, strategy training, to address stroke survivors’ individually tailored participation-related goals (Skidmore, 2011). The purpose of this descriptive case series was to refine the iADAPTS mobile health application and strategy training intervention protocol to be delivered remotely. We also aimed to assess the safety of delivering strategy training remotely using the iADAPTS mobile health system. Community-dwelling people (n=5) with chronic stroke, prior exposure to strategy training, and access to a mobile device completed 1 in-person intervention session and 5 weeks of remote intervention to address their goals. Two key revisions to the iADAPTS application were based on feedback from participants: 1) the number of active buttons per screen was limited, to make clear the participant’s next step in the intervention; and 2) words, rather than icons, were used to indicate the purpose of buttons. The intervention protocol was refined to delineate guiding principles to goal setting that may facilitate the iterative nature of the intervention without hindering participants’ progress toward the goal. The therapist contacted participants to discuss safety on 7 of 34 activity trials, prior to participants carrying out activities. In all cases, a safe plan was established and no adverse events (e.g., falls) occurred during the study. This work represents a first step toward establishing the use of mobile health interventions with meta-cognitive rehabilitation interventions. Future work should establish the efficacy and effectiveness of mobile health approaches to intervention. This will support development of integrated rehabilitation models that can promote ongoing access to specialized neurorehabilitation services among populations that have limited access to these services.
Introduction
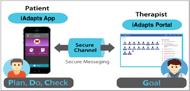
The iADAPTS mobile health system was developed to support strategy training. Strategy training is a rehabilitation intervention in which participants are trained to self-identify a goal, create a plan to achieve this goal, carry out the plan, and then self-reflect to identify strategies that worked and/or different approaches to the same goal (Skidmore, 2011, 2015). The participant then incorporates the new approaches to create another plan and continues in this manner until the goal is met. Strategy training is traditionally delivered in-person, guided by a workbook. The iADAPTS mobile health system contains: 1) iADAPTS mobile health application, 2) iADAPTS web-based clinician portal, and 3) real-time, two-way participant-therapist communication via a secure channel (Figure 1). The integration of the iADAPTS mobile health system across in-person and remote intervention sessions may facilitate ongoing access to specialized rehabilitation services in regions with limited access to these specialized services (e.g., rural regions). The specific aims of this study were to:
- Refine the iADAPTS mobile health application to support remote strategy training.
- Adapt the strategy training intervention protocol for delivery remotely.
- Assess the safety of delivering strategy training remotely.
Methods
We conducted a sequential descriptive case series (n=5) to allow for iterative revision of the iADAPTS mobile health system and intervention.
Participants
Community-dwelling people with chronic stroke (≥6 months post-stroke) who: 1) were previously exposed to strategy training intervention within our laboratory, 2) were able to read words on a mobile device (participant self-report), and 3) had access to a personal mobile device (e.g., iOS or Android smartphone or tablet) were recruited for the present study. Participants were excluded if they had poor awareness of deficits an impact of these deficits on daily activities (measured by Self Awareness of Deficits Inventory) or resided greater than 100 miles from Pittsburgh, Pennsylvania. All participants provided written informed consent.
Intervention
Participants were engaged in 1 in-person intervention session to review the strategy training approach that they had been exposed to during a previous study (NCT01934621). The Canadian Occupational Performance Measure was completed to identify the participant’s current participation-related goals. The iADAPTS mobile health application was uploaded to the participant’s device and they were oriented to the application. A telephone call was scheduled with the therapist (EK) within the next week to identify and resolve any technology difficulties the participant may be experiencing. Participants were not instructed to use the application a specific number of times per week. If the participant asked for a specific frequency the therapist indicated that we anticipated they would use the application 3 times per week. Participants were asked to use the iADAPTS application for 5 weeks. The intervention therapist monitored the participants’ goals and plans for safety in iADAPTS clinician portal and remained available to participants via the messaging function in the application and via telephone during this time. If there was an extended period of inactivity in the application, the therapist reached out to the participant via in-application message and telephone to identify and resolve barriers to application use.
Outcomes
Narrative intervention notes, a participant interactions log, and audio-recorded telephone calls informed adaptations to the iADAPTS application and the remote intervention. Participants’ perspectives of the iADAPTS application were assessed using the Post-Study System Usability Questionnaire (PSSUQ). Participants’ perspectives of the remote intervention were assessed using the Client Satisfaction Questionnaire-8 (CSQ). Safety of remote intervention was assessed by monitoring adverse events that occurred while the participant was carrying out a plan (e.g., falls). We also monitored the number of times the therapist intervened to discuss safety concerns.
Analyses
Participant characteristics and sums of the PSSUQ and CSQ are reported individually. Count data are reported for the number of goals, adverse events, and safety-related therapist-participant interactions.
A design team meeting was held upon completion of intervention with participants 1 through 3. Revisions to the iADAPTS application were made and the new version of the iADAPTS application was deployed during intervention with participants 4 and 5. The clinical team, occupational therapists with expertise in strategy training, monitored and refined remote intervention approaches with each participant.
Results
Participants
We contacted 21 participants who had previous exposure to strategy training through our research laboratory. Our initial, conservative, criteria excluded individuals with a history of falls. Ten participants completed the telephone screen and 2 were included. Eight were excluded due to: falls or loss of balance (7) and no personal device (1). As falls are common among people with stroke and these people may benefit from strategy training, we re-examined our exclusion criteria. A panel of clinicians with expertise in stroke rehabilitation determined that people with impaired self-awareness may be at greater risk for injury during remote strategy training than those with a history of falls. Thus, our criteria were adjusted to exclude people with poor self-awareness of current deficits and/or the impact of current deficits on daily activities. Those with history of falls were eligible to participate. We contacted 3 of the participants who were previously deemed ineligible due to falls or loss of balance and all 3 were deemed eligible for the study.
Participant |
1 |
2 |
3 |
4 |
5 |
|
|---|---|---|---|---|---|---|
Age |
81 |
67 |
69 |
57 |
67 |
|
Gender |
M |
F |
F |
F |
F |
|
Race |
Caucasian |
Caucasian |
Caucasian |
African-American |
Caucasian |
|
Education |
Bachelors |
High School |
Associates |
High School |
Bachelors |
|
Stroke Type |
Ischemic |
Ischemic |
Ischemic |
Hemorrhagic |
Ischemic |
|
Stroke Hemisphere |
Right |
Left |
Right |
Right |
Bilateral |
|
Chronicity (Years) |
2.36 |
2.91 |
1.10 |
2.31 |
3.27 |
|
Mood (PHQ-9)a |
1 |
4 |
2 |
2 |
3 |
|
Executive Functions |
9 |
5 |
11 |
10 |
12 |
|
Language (RBANS Index |
85 |
101 |
101 |
90 |
92 |
|
Attention (RBANS Index)c |
91 |
88 |
82 |
60 |
49 |
|
Immediate Memory (RBANS Index)c |
100 |
90 |
100 |
106 |
61 |
|
Delayed Memory (RBANS Index)c |
110 |
102 |
106 |
99 |
48 |
|
Visuospatial (RBANS Index)c |
58 |
78 |
100 |
58 |
64 |
|
Motor Function (CMA)d |
33 |
36 |
28 |
16 |
23 |
|
Client Satisfaction Questionnaire-8 |
25 |
32 |
30 |
30 |
28 |
|
Post-Study System Usability Questionnairee |
86 |
38 |
35 |
31 |
73 |
|
Number of Activity Trials |
2 |
14 |
4 |
12 |
2 |
|
aRange is 0 to 27, low scores are low depressive symptoms; bMean=10, SD=3; cMean=100, SD=15; dRange is 6 to 42. Low scores are more impaired motor function.eRange is 0-133, low scores indicate high usability. |
|
|||||
Participant characteristics are described in Table 1. Participants ranged in age from 57 years to 81 years. Four were female. Four participants with ischemic stroke and one had hemorrhagic stroke. Our sample had a combination of right (3), left (1), and bilateral (1) stroke at the cortical (2) and sub-cortical (3) level. Participants were 1.10 to 3.27 years post-stroke. No participants were concurrently participating in rehabilitation therapies.
Scores on cognitive, motor, and affective assessments reflect participants’ function at 6-months post-stroke (assessments were conducted during the original strategy training study, NCT01934621). Participants had a range of impairments in executive functions (DKEFS Trail Making Condition 4 vs. DKEFS Trail Making Condition 5 scaled scores, range 5 to 12), attention (RBANS Attention Index Score, range 49 to 91), and visuospatial skills (RBANS Visuospatial Index Score, range 58 to 100). All participants had intact language (RBANS Language Index Score, range 85 to 101). Most participants had intact immediate and delayed memory, however, one participant had marked impairment in these domains (RBANS Immediate Memory Index Score, range 61 to 106, RBANS Delayed Memory Index Score, range 48 to 110). Our sample had low depressive symptoms (PHQ-9, range 1 to 4), and a range of motor impairments (Chedoke McMaster Stroke Assessment, range 16 to 36).
Outcomes
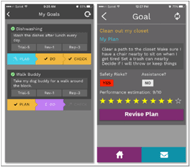
The therapist’s approach to facilitating goal setting was refined, with careful attention to the size of goals set during intervention. If participants identified a broad goal, they were encouraged to break the goal down into smaller individual goals. If the goal required multiple iterations of the same task (e.g., cleaning out multiple closets), the participant was encouraged to identify a specific rate to check in on their progress and repeat the plan.
Of the 34 activity trials completed during the study, the intervention therapist contacted participants to discuss the safety of 7 plans prior to approving them. In each case, participants identified that they had a safe plan in place that was not detailed in the plan that was entered in the iADAPTS application. Each of the 7 plans was subsequently carried out safely. No adverse events occurred during this study.
Participants identified high satisfaction with the intervention (Client Satisfaction Questionnaire-8, range 25 to 32 of 32). Participants’ rating of system usability ranged (Post-Study System Usability Questionnaire, range 31 to 86 of 133, low is better).
Conclusions
The purpose of this study was to refine the iADAPTS mobile health system and remote intervention procedures in preparation for integration into strategy training intervention. We also aimed to identify if strategy training could be delivered remotely using mobile health technology, promoting access to ongoing specialized neurorehabilitation for people with limited access to these services (e.g., rural populations). We identified that the iADAPTS mobile health system could be safely used to deliver strategy training remotely.
To our knowledge, the iADAPTS mobile health system is the first mobile health system that was developed to support an iterative rehabilitation intervention. Our study design limited the ability to assess efficacy or effectiveness of this intervention approach. Future studies that optimize models for integration of mobile health systems within rehabilitation, examine the efficacy and effectiveness of these models, and explore the cost-effectiveness of integrated rehabilitation models will advance this work.References
Kamal, A.K., Shaikh, Q., Pasha, O., Azam, I., Islam, M., Memon, A.A., et al. (2015). A randomized controlled behavioral intervention trial to improve medication adherence in adult stroke patients with prescription tailored Short Messaging Service (SMS)-SMS4Stroke study. BMC Neurol,15(1):212.
Laver, K., George, S., Thomas, S., Deutsch, J.E., & Crotty, M. (2014). Virtual reality for stroke rehabilitation. Stroke, 43(2)e20-1.
Skidmore, E.R., Holm, M.B., Whyte, E.M., Dew, M.A., Dawson, D., & Becker, J.T. (2011). The feasibility of meta-cognitive strategy training in acute inpatient stroke rehabilitation: Case report. Neuropsychol Rehabil, 21(2):208-23.
Skidmore, E.R., Dawson, D.R., Butters, M.A., Grattan, E.S., Juengst, S.B., Whyte, E.M., et al. (2015). Strategy training shows promise for addressing disability in the first 6 months after stroke. Neurorehabil Neural Repair, 29(7):668-76
Acknowledgements
Funding sources: R01 HD07469; 90RE5018.