Asia Khaton1, Genevieve Daoust1,2, Resi Contardo2, Paula W. Rushton1,2,
1University of Montreal, 2Marie-Enfant Rehabilitation Center (Montreal, Canada)
INTRODUCTION
Children with Cerebral Palsy (Gross Motor Function Classification System [GMFCS] levels IV and V) do not have the motor skills to independently crawl, walk or propel a manual wheelchair [1]. Thus, they miss important self-mobility experiences necessary to acquire cognitive and psychosocial skills. One means of enabling self-produced locomotion for this population is through the use of power mobility, which has been shown to improve cognitive and perceptual skills and increase participation with their peers in everyday activities [2]. Despite the positive impacts of power mobility on developmental milestones, it is rarely introduced in the preschool years for children with severe impairments [3]. To promote its early introduction for children with severe impairments, a new training program entitled Initiating Power Mobility Training Among Young Children was recently developed. The primary objective of this study was to explore the effect of this newprogram on the acquisition of 4 foundational power mobility skills (cause-and-effect, stop-and-go, directional control and independent travel). The secondary objective of the study was to explore its effect on mobility related to participation, mastery motivation, social interaction and cognition.
METHODS
Design
This study used a single-subject multiple-baseline across participants design.
Participants and setting
We studied 3 volunteer parent-child dyads that were followed in the Communication and Assistive Technology Program at a pediatric rehabilitation center. Children were aged 25, 33 and 34 months. All had cerebral palsy with a GMFCS level of IV and were dependant on an adult for mobility. None of them had experience using power mobility prior to the study. Informed consent was obtained from all participants.
Outcome measures
Quantitative data
- Foundational Power Mobility Skills - Four fundamental skills (i.e., cause-and-effect, stop-and-go, directional control and independent travel) were assessed using a 4-point response scale (0 = does not attempt the ability to 4 = demonstrates the ability without physical help or prompt more than 90 % of the time).
- Power Mobility Screen (PMS) - assessed cognitive (7 items) and motor (10 items) driving skills for children who have multiple, severe impairments and who use either a joystick or switch(es) to access a power mobility device [4]. It is scored on a 4-point response scale (0=no attempt to 3=consistent in completing task).
- The Pediatric Evaluation of Disability Inventory–Computer Adaptive Test (PEDI-CAT) - measured abilities in three functional domains: daily activities, mobility and social/cognitive [5]. It rates each item on a 4-point response scale (0=unable to 4=easy). Only the Mobility and Social/Cognitive domains in the PEDI-CAT Speedy version were completed for the study.
- Dimension of Mastery Questionnaire (DMQ) preschool version - a caregiver report that assessed both the instrumental and expressive aspects of mastery motivation on a 5-point scale (1= “Not at all like this child to 5= “Exactly like this child) [6].
- Control Measure - the number of triangular shaped forms successfully placed on a board within 2 minutes.
Qualitative data
- Reinforcement Assessment for Individuals with Severe Disabilities (RAISD) – collected data via structured interview with a caregiver regarding various categories of stimuli (visual, auditory, tactile, kinesthetic) that could be used as reinforcers for each participant in the intervention.
- Qualitative Semi-Structured Interview – collected data pre- and post training regarding the parent’s perception of the power mobility training process, their expectations and their concerns. Interviews were recorded for qualitative data analyses.
- Logbook – used to compile data at every session regarding goals and training session information (e.g., switch site, level of cooperation of the child, problems occurred, people present during training).
Equipment
The power mobility device (PMD) used was an Invacare TDX SP with MK IV electronics and ASL control interface. Round switches were chosen due to the small amount of force needed for activation, less fine motor skills needed and auditory feedback when activated. Two types of switches were use depending on the mounting location. AbleNet SPECS switch were mounted on the headrest (i.e Stealth Ultra or Ottobock three pad headrest) and Ablenet Buddy Button switches were mounted on a tray for upper extremities access. The child custom multi-adjustable seating system from their stroller was installed on the PMD with straps to ensure a better body alignment and sitting posture.
Procedure
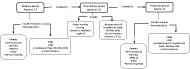
Analysis
RESULTS
Switch control changed over the course of the intervention as the children mastered more driving skills. While all children started with hand access on a tray, they finished with 1-2 switches mounted on the headrest and 1-2 switches mounted on the tray for better motor accuracy.
The number of triangular shaped forms successfully placed on a board within 2 minutes (i.e., control measure) remained none across all time points.
All 3 children demonstrated a trend of improvement in all 4 foundational skills. The skills of cause-and-effect and independent travel were accomplished (score of 4) by all 3 children by the end of training. The level of achievement of the stop-and-go and directional control skills varied among children and fluctuated for one child.
DISCUSSION
This multiple single subject research project explored the effectiveness of the Initiating Power Mobility Training Among Young Children program with three preschool, severely impaired children and their mother. Improvement in all 4-power mobility foundational skills and in PMS scores post-intervention suggests the effectiveness of this training program and highlights the capacity of pre-school children with severe mobility limitations to participate in a power mobility training program. Our findings confirm that of previous studies [7-9]. It also showed how parental perception can be modified regarding the introduction of power mobility at such an early age and the associated benefits for their child when involved in training. Additionally, this program highlights the effectiveness of certain training methods such as free exploration using turning function only, the incorporation of play in stop-and-go learning using the most reliable site for switch activation (i.e., head or hand) and in goal-directed mobility.
| Child A | Child B | Child C | ||||
|---|---|---|---|---|---|---|
| Measure | Pre | Post | Pre | Post | Pre | Post |
| The Power Mobility Screen | ||||||
| Cognitive Scale | 8/21 | 16/21 | 12/21 | 16/21 | 11721 | 18/21 |
| Motor Scale | 10/30 | 17/30 | 15/30 | 20/30 | 18/30 | 20/30 |
| Total Score | 18/51 | 33/51 | 27/51 | 36/51 | 29/51 | 38/51 |
| PEDI-CAT ("Speedy") | ||||||
| Mobility Score | 46 | 42 | 41 | 46 | 50 | |
| Social/Cognitive Score | 53 | 50 | 52 | 52 | 53 | |
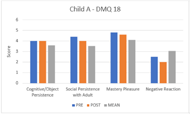
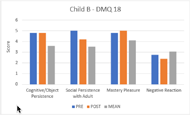
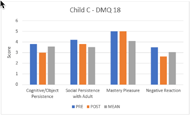
Results are contradicting in the DMQ-18. On one side, all three children exhibited lower scores in negative reaction subscales post-intervention, which means they expressed less negative reactions to failure. On the other side, they also all showed lower scores on the social persistence post-intervention reflecting lower perseverance with social interactions with adults. Scores also varied among children regarding cognitive/object persistence and mastery pleasure
There were a number of study limitations, for instance the short time frame between pre- and post-assessment may have impacted the results for some measures. In terms of functional skills, no clinically relevant improvement was seen in the PEDI-CAT score post-intervention. Nevertheless, Child B and Child C showed improvement in the social and cognitive domain in terms of communicating with others, which could be a benefit from the power mobility training as described by other studies [7-9]. Finally, because of the study design used and the small sample, the level of evidence for the effect of the training program can’t be generalized to all children with severe physical impairments.
CONCLUSION
As the literature encourages the introduction of power mobility for young children with severe motor impairment, the type of training methods remains undefined. This initial research with severely impaired preschoolers can help to build evidence in the development of a more valid training program for pre-schoolers with severe impairments.REFERENCES
[1] Palisano, R. J., Rosenbaum, P., Bartlett, D., & Livingston, M. H. (2008). Content validity of the expanded and revised Gross Motor Function Classification System. Developmental Medicine & Child Neurology, 50(10), 744-750.
[2] Rosen, L., Arva, J., Furumasu, J., Harris, M., Lange, M. L., McCarthy, E., ... & Sabet, A. (2009). RESNA position on the application of power wheelchairs for pediatric users. Assistive Technology, 21(4), 218-226.
[3] Livingstone, R., & Field, D. (2014). Systematic review of power mobility outcomes for infants, children and adolescents with mobility limitations. Clinical rehabilitation, 28(10), 954-964.
[4] Bundonis, J. (2008). Pediatric Power Mobility Assessment and Training. Temple, TX: Communicate & Negotiate, LLC.
[5] Dumas, H. M., Fragala-Pinkham, M. A., Rosen, E. L., Lombard, K. A., & Farrell, C. (2015). Pediatric evaluation of disability inventory computer adaptive test (PEDI-CAT) and Alberta infant motor scale (AIMS): Validity and Responsiveness. Physical therapy, 95(11), 1559-1568.
[6] Morgan, G. A., Liao, H. F., Nyitrai, Á., Huang, S. Y., Wang, P. J., Blasco, P., ... & Józsa, K. (2017). The revised Dimensions of Mastery Questionnaire (DMQ 18) for infants and preschool children with and without risks or delays in Hungary, Taiwan, and the US. Hungarian Educational Research Journal, 7(2), 48-67.
[7] Jones, M. A., McEwen, I. R., & Neas, B. R. (2012). Effects of power wheelchairs on the development and function of young children with severe motor impairments. Pediatric Physical Therapy, 24(2), 131-140.
[8] Kenyon, L. K., Farris, J., Brockway, K., Hannum, N., & Proctor, K. (2015). Promoting self-exploration and function through an individualized power mobility training program. Pediatric Physical Therapy, 27(2), 200-206.
[9] Furumasu, J., Guerette, P., & Tefft, D. (1996). The development of a powered wheelchair mobility program for young children. Technology and Disability, 5(1), 41-48.