STANCE CONTROL ORTHOTIC KNEE JOINT UTILIZING ANKLE MOTION CONTROL
ABSTRACT
A Stance Control Orthotic Knee Joint (SCOKJ) refers to the application of a mechanically locking device that resists knee flexion upon limb support when a flexion moment about the knee is created. Currently no mechanical control system that activates the lock/unlock mode of the knee joint allows for independent lock and release sequences based on tracking the Range of Motion (ROM) that is occurring about the ankle joint. This paper will describe a system that will accomplish this function.
BACKGROUND
Traditionally patients with weak or absent knee musculature were restricted to a knee joint that held them in a static position during standing and gait. The SCOKJ was developed to create knee stability when required but yet allow for flexion to normalize gait patterns. In the past several years four commercial manufacturers have developed SCOKJ's. Two versions are currently available (Horton Labs, Otto Bock)and the others are to be released soon (Fillauer, Becker). Horton Labs describes their new electronic module control device as a "work in progress" (1).
Currently there are variations of control methods to lock/unlock the knee mechanism which range from electronic foot sensors, weight bearing mechanical switches, push/pull cables, and gravity systems. These are used in conjunction with a variety of locking mechanisms. For the purpose of this paper our work focuses on the control methodology. The goal is to develop a simple mechanical system that is durable, easily maintainable and applied, and relatively inexpensive.
To create a dynamic control method that will allow the user to have their knee positively locked at times where a flexion moment is created about the knee axis, and unlocked while the knee is inherently stable or in non-weight bearing free swing. This kinematic relationship between body positioning and locking control should be easily adapted for each patient's gait characteristics. Currently, all mentioned attributes are not available in one system. We will demonstrate a system that shows good potential in obtaining these goals. Two patient trials have proven this technology can work.
STATEMENT OF PROBLEM
The object of this study is to determine if a SCOKJ can be effectively controlled through a method of tracking the ROM about the ankle joint. If so, can the locking/unlocking control be adjusted independent from each other and be fine tuned to match the unique gait characteristics of the individual patient.
DESIGN
This project created several lab models which resulted in the manufacturing of two prototype orthotic systems that have been field tested to validate concept. The latest designs will be described here.
A custom molded acrylic knee-ankle-foot-orthosis (KAFO) was manufactured to our patient's leg model and a Horton SCOKJ was applied which utilizes a dual push/pull cable controlling a locking cam at the joint axis. Double action ankle joints were formed into a molded foot shell (any type ankle joint that allows ROM will work). Spring assists were used for posterior channels (dorsi-assist) and locking pins in the anterior (dorsi-resist). To this KAFO we installed our control system.
CONTROL SYSTEM
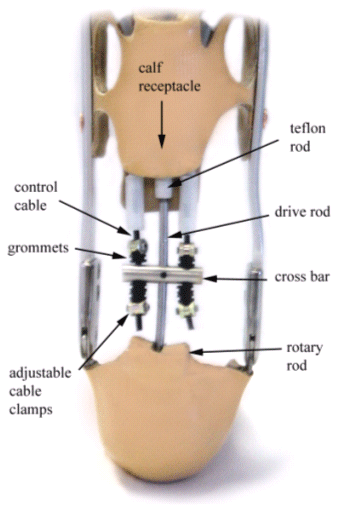 To the upper calcaneal border of the foot shell a 3/8"
diameter x 1" length steel rod (rotary rod) with a thread tapped through
the longitudinal center was laminated into the foot section so that it
could rotate freely. A channel was cut at the location of the rotary rod
center to allow access and movement. A 3/16" x 4" rod (drive rod) threaded
on both ends was installed through the channel into the rotary rod so
that it is perpendicular and faces upward. To the other end a threaded
Teflon rod (11/32" diameter x 1 ½" length) is attached and a 3/8" receptacle
is formed vertically in the center posterior calf section. Therefore,
the vertical (drive rod) is attached at one end to the foot shell rotary
rod, and proximally slides into the calf receptacle. As the foot plantar-flexes,
the "drive rod" moves upward into the receptacle, and is pulled downward
during dorsi-flexion. This then tracks the motion that is occurring about
the ankle axis. To the posterior "drive bar" a 3/8" x 1 ¼" "cross bar"
drilled through the longitudinal center with a set screw was slipped over
the "drive bar" and affixed at the middle. Two holes were then drilled
on either side of the "cross bar" that would allow the control cables
to freely pass through. To the cable, adjustable clamps were attached.
The cable can travel through the "cross bar" and be resisted by the clamps
at points determined by the clinician to create a push or pull of the
cable. Therefore, by plantar-flexing the foot, the "drive rod" is driven
upwards with the cable moving through the "cross bar" until it comes into
contact with the cable clamp which then pushes the cable upwards, activating
the cam which locks the knee. Conversely, by dorsi-flexing the ankle the
cable slides through the "cross bar" till it contacts the lower cable
clamp which pulls the cable, disengages the locking cam, and allows free
knee flexion. The control sequence therefore is adjustable based on the
position of the cable clamps.
To the upper calcaneal border of the foot shell a 3/8"
diameter x 1" length steel rod (rotary rod) with a thread tapped through
the longitudinal center was laminated into the foot section so that it
could rotate freely. A channel was cut at the location of the rotary rod
center to allow access and movement. A 3/16" x 4" rod (drive rod) threaded
on both ends was installed through the channel into the rotary rod so
that it is perpendicular and faces upward. To the other end a threaded
Teflon rod (11/32" diameter x 1 ½" length) is attached and a 3/8" receptacle
is formed vertically in the center posterior calf section. Therefore,
the vertical (drive rod) is attached at one end to the foot shell rotary
rod, and proximally slides into the calf receptacle. As the foot plantar-flexes,
the "drive rod" moves upward into the receptacle, and is pulled downward
during dorsi-flexion. This then tracks the motion that is occurring about
the ankle axis. To the posterior "drive bar" a 3/8" x 1 ¼" "cross bar"
drilled through the longitudinal center with a set screw was slipped over
the "drive bar" and affixed at the middle. Two holes were then drilled
on either side of the "cross bar" that would allow the control cables
to freely pass through. To the cable, adjustable clamps were attached.
The cable can travel through the "cross bar" and be resisted by the clamps
at points determined by the clinician to create a push or pull of the
cable. Therefore, by plantar-flexing the foot, the "drive rod" is driven
upwards with the cable moving through the "cross bar" until it comes into
contact with the cable clamp which then pushes the cable upwards, activating
the cam which locks the knee. Conversely, by dorsi-flexing the ankle the
cable slides through the "cross bar" till it contacts the lower cable
clamp which pulls the cable, disengages the locking cam, and allows free
knee flexion. The control sequence therefore is adjustable based on the
position of the cable clamps.
EVALUATION
This control mechanism worked as intended with our two subjects. It was able to lock reliably upon heel strike, and release at the adjusted dorsi-flexion angle set for pre-swing.
DEVELOPMENT
The goal is to improve upon design for better ease of clinical usage and manufacturing processes. In the future, this control mechanism will be tested with various ankle componentry and molded designs. An LED will be installed for visual observation to identify when the knee locks and releases.
DISCUSSION
Further work will be done with pathokinesiology in order to more closely determine ideal locking/unlocking points as it relates to the gait cycle. This information will then become a base point. We feel it is important that the clinician then has the freedom to customize these dynamics to better individualize them to meet the patients' needs
ACKNOWLEDGEMENTS
This study was funded by the National Institute on Disability and Rehabilitation Research grant # H133E003001.
The author thanks Pierre Leung, B.S. and Adrian Polliack, Ph.D. for their support and consult, Jacqueline Perry, M.D. for her review and advice, and Horton Technologies for supplying knee joints and consult.
Roger B. Weber, CPO,
RERC on Technology for Children with Orthopedic Disabilities
7503 Bonita Street
Downey, CA 90242
(562) 401-7994, (562) 803-6117 (fax)
rweber@ranchorep.org
