Reduce Skin Temperature Elevation Using an Alternating Ischial Support Wheelchair
ABSTRACT
Sitting without pressure relief in a wheelchair for extend time periods can lead to skin temperature elevation and potentially pressure ulcers (PU). Skin temperature has been shown to be an effective measure of incipient PU formation. Therefore, by reduced skin temperature elevation, the occurrence of PUs can be lessened. A new seating design in which the ischial and back supports can be adjusted was applied to a wheelchair. Alternating the supports provides a type of pressure relief regiment. The effectiveness of this design at preventing skin temperature elevation was tested. It was shown that skin temperature experiences smaller increases when using the system compared to sitting in a standard posture and performing manual pressure releases at intervals, particularly in the ischial region. Furthermore, the manual pressure relief maneuver could not be sustained long enough to provide full relief.
KEY WORDS:
Skin Temperature, Wheelchair, Posture
INTRODUCTION
Sitting for extended time periods in a wheelchair leads to excessive pressure over the ischial tuberosities and coccyx (1), which significantly increases the risk of PU. It has also been suggested (2) that factors such as moisture and high temperature may increase susceptibility to PU in wheelchair-bound individuals. A rise in skin temperature may increase the metabolic demands of the cells in a region already suffering from poor circulation due to pressure. Elevated skin temperatures are accepted indicators of incipient ulcer formation (3).
A new seat design which allows for decreased ischial support and increased lumbar support was proposed by Makhsous et al. (4). This chair design permits the back part of the seat (BPS) to tilt downward 20° with respect to the front part of the seat (FPS). Additionally, the backrest of the chair can be inflated to provide increased lumbar support. The postural benefits reported (4) could potentially benefit wheelchair users. More importantly, adapting this design to a wheelchair introduces a new method of relieving sitting pressure for wheelchair users. Two postures can be achieved with the chair design. The Normal posture involves no increased lumbar support with full ischial support. The WO-BPS posture includes full lumbar support and drops ischial support (BPS) by 20°. These adjustments can be automated through the use of a programmed controller, a motor, and a vacuum pump. Automation eliminates the need for wheelchair users to perform manual pressure releases and allows for accurate measurement of results.
The purpose of this study was to explore the effects of the new seating concept on skin temperature elevation in areas susceptible to PUs. Additionally, sitting alternately between Normal and WO-BPS postures, defined an Alternate protocol, will be compared to sitting in the Normal plus the clinically recommended Push-up routine, defined as Normal+Push-up protocol.
METHODS
A wheelchair with adjustable lumbar and ischial supports was used (4). A motor controlled the angle of the BPS, which could be tilted 20 ° downwards with respect to the front part of the seat. An air bladder installed in the backrest could be inflated through the use of a vacuum pump to provide lumbar support. To ensure that the same levels of support were achieved in each trial, a Programmable Logic Controller (Vision230 OPLC, Unitronics Inc., Quincy, MD) was programmed to control both the pump and motor and was used to change the postures.
Twenty able-bodied office workers (36.60 ± 13.24 years old; 71.89 ± 17.74 kg; 169.27 ± 13.24 cm) were tested in this laboratory setup. Informed and written consent following the guidelines of the Institutional Review Board was obtained before any experimentation.
Semiconductor thermometers (Thermometrics, Inc., NJ, USA) were placed on the skin to measure local skin temperature. Three pairs of thermometers were placed on the skin under both the right and left legs at the ischial tubersoity (IT), posterior proximal thigh (PT), and posterior middle thigh (MT). The readings of thermometers were acquired using a data acquisition system (DAQCard 6036E, National Instruments, TX) at 100Hz. Temperature was measured in degrees Celsius, and data was collected over two 60-minute trials of which the first trial was randomly chosen. In the Alternate trial the seat posture changed from Normal to WO-BPS at ten-minute intervals. In the Normal+Pushup trial the chair was kept at the Normal position during which the subject performed a clinically recommended push-up every 20 minutes. A push-up entails the subject grabbing both handles of the chair and lifting themselves out of the chair. In between trials the subject stood up to create a zero pressure environment that would allow temperatures to return to standing levels.
Comparisons between the Alternate and Normal+Push-up protocols were computed at each thermometer location. A paired t -test was used to detect significances between the trials with a significance level set at 0.05.
RESULTS
Fig. 1 shows a typical results from one subject. The differences between the two trials are evident, especially under the IT where the increase in temperature was much less during the Alternate trial. During the Normal+Pushup trial, each push-up only slightly lowered skin temperature for a brief time period 48.5 ± 15.5 seconds , leaving the skin temperature continually increases throughout the entire trial. During the Alternate trial, the skin temperature increased soon after the subject sit down and kept slow trend of increase thereafter. As soon as the Alternate posture changing started, 10 min after the start of the trial, temperature elevation was largely under control, particularly under the IT.
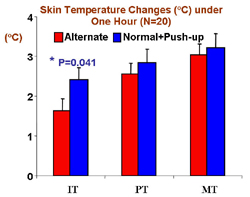
Average results across the group of subjects are given for IT, PT and MT in Fig. 2. For both trials, skin temperature was significantly (P<0.001) increased from the reading of standing, however, lower elevation was seen for all the recording sites from Alternate protocol, with significance found under the IT (1.6 ± 0.3 vs. 2.41 ± 0.3 ° C; P =0.041). No significant differences were detected between the two trials at the PT and MT.
 |
|---|
DISCUSSION
Both from the postural benefits demonstrated by Makhsous et al. (4) and the results from the present study, the new seating system presents itself as a potential solution in preventing PUs. As previously mentioned, the currently accepted pressure relief regime is for a wheelchair user to complete a push-up out of their seat. As seen in Fig. 1, the push-up does not help to change the trend of skin temperature elevation. On the other hand, the Alternate trial can allow for a much longer pressure relief and the results demonstrated this. The Alternate trial provided less skin temperature elevation without the need for the subject to perform a pressure release manually (Fig. 2). The postural change allows enough relief over the IT to provide lessened skin temperature elevation than a push-up regiment. The lumbar support keeps the user from sinking as the ischial support is lowered. This allows for decreased pressure and increased air flow for long periods of time in the ischial region, both of which lead to lowered skin temperature elevation. In order to further validate this design, studies must be completed on actual wheelchair users who are at risk for PUs. The postural changes will be more difficult for a spinal cord injury patient to adapt to due to the increasd load on the anterior thighs and hips. Moreover, the ten minute duration of the WO-BPS posture, currently used in the Alternate trial, is an arbitrary period of time that can be further explored and optimized.
REFERENCES
- Staas, W.E. and H.M. Cioschi, Pressure sores - a multifaceted approach to prevention and treatment, In: Rehabilitation medicine. Adding life to years (Special Issue). West J Med, 1991. 154: p. 539-44.
- Maureen, A.L. and S.H. Sprigle, Skin Temperature Measurement to Predict Incipient Pressure Ulcers. Center for Rehabilitation Technology, Helen Hayes Hospital, NY, 2002.
- Shea, J.D., Pressure sores: classification and management. Clin Orthop, 1975. 112: p. 89-100.
- Makhsous, M., Lin, F., Hendrix, R., Hepler, M., Zhang, L., Sitting with Adjustable Ischial and Back Supports: Biomechanical Changes , Spine, 2003. 28: p. 1113-1122.
ACKNOWLEDGEMENTS
The project was supported in part by PVA (Paralyzed Veterans of America) Award #2321-01, and Falk Medical Research Trust.
Author Contact Information:
Mohsen Makhsous, PhD,
Rehabilitation
Institute of Chicago,
345 E. Superior St.,
Chicago, IL 60611,
Office Phone
312-238-4824,
EMAIL: m-makhsous2@northwestern.edu

