EFFECT OF MUSCLE FATIGUING TASKS ON SUBACROMIAL SPACE IN MANUAL WHEELCHAIR USERS
Yen-Sheng Lin, MS; Alicia Koontz, Ph.D. RET, Lynn Worobey, BS; Michael Boninger, MD
1Human Engineering Research Laboratories, VA Pittsburgh Healthcare System 2Department of Rehabilitation Science and Technology, University of Pittsburgh, Pittsburgh, PA 3Department of Bioengineering, University of Pittsburgh, Pittsburgh, PA 4Department of Physical Medicine and Rehabilitation, University of Pittsburgh, PA
INTRODUCTION
Manual wheelchair users are at high risk for shoulder impingement syndrome due to repetitive wheelchair propulsion and transfer. Shoulder muscle fatigue is a common consequence of overuse and may lead to the development of shoulder impingement syndrome (Cohen & Williams, 1998; Rodgers et al., 1994) . Impingement occurs when the rotator cuff (RC) tendons become compressed and irritated as they pass through the sub-acromial space, which is an area located above the head of the humerus and below the acromion. A deficiency in the RC muscles reduces their ability to stabilize the humeral head against the glenoid cavity of the scapula causing migration of the humeral head into the space. Superior humeral head migration was found after RC muscle fatigue (Chopp, O'Neill, Hurley, & Dickerson, 2010). Although the amount of humeral translation may be considered small (on the order of 1 to 3mm), the compressive effects on the subacromial structures are significant due to the limited size of the subacromial space. While electromyography (EMG) confirmed signs of local muscle fatigue for several shoulder girdle muscles, the infraspinatus muscle was fatigued to a greater extent. (Chopp, et al., 2010).
Ultrasound offers many advantages over traditional methods (e.g. radiography and MRI) to measure the space such as portability, real-time, non-invasive, and radiation-free measurement. Ultrasound has been used successfully to measure a decrease of acromiohumeral distance (AHD), the linear measure of subacromial space, in studies of healthy able-bodied subjects with and without impingement (Royer et al., 2009; Teyhen, Miller, Middag, & Kane, 2008) . Wheelchair users represent a unique population for studying AHD due to the types of activities that they routinely perform and their predisposition to developing shoulder impingement.
A previous study investigated two types of fatigue protocols in able-bodied subjects: a global shoulder fatigue protocol that simulated job tasks and a local fatigue protocol that targeted the shoulder external rotators and was associated with known scapular orientation changes (Chopp, Fischer, & Dickerson, 2011; Tsai, McClure, & Karduna, 2003) . The global protocol induced injury-like changes in humeral head translation and scapular orientation changes in an ‘impingement sparing’ direction. They concluded that translation, not altered scapular kinematics, is the dominant mechanism creating reductions in the subacromial space consistent with impingement. While this study simulated job tasks to elicit shoulder fatigue, wheelchair users perform many daily functional tasks involving large weight-bearing forces and awkward shoulder positions. The purpose of this study was to examine the effects of repetitive weight-relief raises (global fatigue) and shoulder external rotation exercise (local fatigue) on the subacrominal space measured using pre-post ultrasound imaging. A second goal was to examine the relationship between subject characteristics, shoulder pain and the AHD. Ultrasonic changes in the AHD resulting from routine weight-bearing activities may be indicative of early stages of shoulder pathology. This research will provide a greater understanding of the mechanisms leading to shoulder impingement in wheelchair users and validate a new measure that can be used to evaluate interventions tailored to preserving upper limb function.
METHODS
Subjects
Twenty-three manual wheelchair users (MWUs) (22 male and 1 female) were recruited. Research protocol was approved by the local institution review board. 16 had a spinal cord injury (5 cervical, 11 thoracic), one had unilateral transfemoral amputation, three had bilateral transtibial amputation, and three had multiple sclerosis. They had no pain in an upper extremity that interfered with normal function and daily activity. The average age (standard deviation) was 46(12) years old, post injury or diagnosis was 15(10) years, and the average height and weight were 178(8) cm and 81(18) kg, respectively. Shoulder pain was assessed with the Wheelchair Users Shoulder Pain Index (WUSPI). Anthropometric measurements of the axillary circumference and upper arm length measured from the most lateral and superior portion of the acromion to the tip of the olecranon were taken on non-dominant side. Surface EMG was used as reference for fatigue onset. Electrodes was placed over the infraspinatus, sternal pectoralis major, and lattismus dorsi using standards previously developed for these muscles (Chopp, et al., 2011). The bi-polar Noraxon Telemyo 2400T electromyography system (Noraxon Inc., Arizona, USA) with 2cm spacing for the dual surface electrodes were placed over the belly of each muscle. A ground electrode was placed on the lateral portion of the clavicle. The raw EMG signals were collected at 1500 Hz and filtered using a 450 Hz low pass cut-off frequency. Ultrasonography was collected using a Philips HD11 1.0.6 ultrasound machine with a 5-12 MHz linear transducer. The same examiner completed all scans for each subject. Baseline ultrasound examination of the AHD was recorded on the non-dominant shoulder. The shoulder was scanned from the anterior aspect of glenoid to the flat segment of posterior scapula to capture the bright reflection of the bony contour of the acromion and humeral head (Figure 1). Video recordings at 60 Hz were captured for each scan.
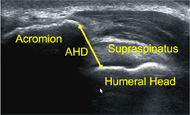 Figure 1. Ultrasonographic image of the acromiohumeral distance in the weight relief raise position d
Figure 1. Ultrasonographic image of the acromiohumeral distance in the weight relief raise position dFatigue Protocols
The first task involved multiple weight relief push-ups (WR) holding up the body weight with an elbow locked position. The second task was a shoulder external rotation (ER) task using the Biodex System 3. These tasks were repeated at a rate of 20 beats per minute with the use of a metronome until the subjects could no longer perform the task due to self-perceived fatigue or for a maximum of 2 minutes. The external rotation task was set for 5% body weight as resistance while internal rotation had a standardized minimum 1-lb resistance. The subjects rested approximately 15 minutes in between the two fatigue protocols. A single ultrasound image was taken at the beginning of the study with the shoulder in a neutral and resting position. Pre-post ultrasound imaging of the AHD was obtained for each task while isometrically holding the weight relief raise position. Muscle activities were collected using EMG for the entire duration of the exercises.
Data Analysis
Each frame of the video was reviewed to determine the narrowest distance of the inferior edge of acromion and humeral head. The AHD was calculated through visual detection of the bony landmarks and the distance computed via a custom Matlab program. The AHD measure was post-processed via an independent rater blinded to the subject testing and timing of the video (e.g. pre or post). Five AHD measurements were considered for the analysis, one baseline AHD with the shoulder in a resting position, two pre-fatigue task AHD measures, and two post-fatigue task AHD measures. To assess reliability of the AHD measure, we compared the two pre-fatigue AHD measurements using the intraclass correlation coefficient (ICC). Local muscle fatigue was confirmed by computing the median power frequency (MPF) and peak amplitude EMG (Luttmann, Jager, & Laurig, 2000). The power spectral density was used to determine the MPF for each 1-second interval over the first 5-second period as pre-fatigue and the last 5-second period as post-fatigue. Changes in MPF were determined by subtracting the averaged post-fatigue MPF values from the averaged pre-fatigue values. The percent change in the peak magnitude of the EMG signal was obtained during the same time interval as the MPF. A paired t-test was used to assess differences in the AHD absolute measures before and immediately after performing WR and ER. Pearson’s correlations between the absolute AHD measures, AHD percentage changes (Equation 1), shoulder pain and demographic data (e.g. height, weight, shoulder circumference, arm length, age, and years since SCI) were examined. Stepwise linear regressions used the baseline AHD in the rest position and demographic variables that were significantly associated with the AHD as independent variables. The dependent variable was the percentage AHD change after each fatiguing task.
AHD percentage change % = (post AHD measure - pre AHD measure)/pre AHD measure ..............................(1)
RESULTS
The results showed high reliability in the baseline AHD measures (ICC coefficient, single measures = 0.73). There were no statistically significant differences in the AHD measures pre-post fatigue for either protocol for the total sample of 23 subjects. However, a trend was found in the percentage change of AHD after repeated weight relief raises (p=0.08) with subjects (n=6) who had signs of infraspinatus EMG local muscle fatigue with a MPF of at least an 8% decrease which was previously regarded as clinically significant (Oberg, Sandsjo, & Kadefors, 1990) (Table 1). Although not significant, a moderate effect size was also found for subjects (n=9) who had confirmed EMG signs of infraspinatus muscle fatigue after the local external rotator protocol (Table 1).
| Muscle | Multiple Weight Relief Raise | Shoulder External Rotation |
|---|---|---|
| Infraspinatus (8% to 20% MPF decrease) | -7.47±8.43 (f2 = 0.90); n=6 | -2.36±7.07 (f2=0.43); n=9 |
| Pectoralis Major & Latissimus Dorsi (8% to 20% MPF decrease) | 0.94±15.63(f2 = 0.02); n=9 | |
| Pectoralis Major & Latissimus Dorsi (Over 20% MPF decrease) | 0.60±4.87(f2 = 0.05); n=4 |
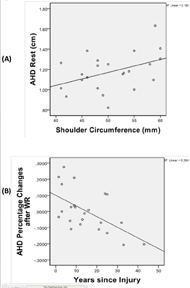 Figure 2. Regression analysis for the AHD (percentage changes after multiple weight relief raises with years since injury) (A) and (neutral shoulder position with the shoulder circumference) (B). d
Figure 2. Regression analysis for the AHD (percentage changes after multiple weight relief raises with years since injury) (A) and (neutral shoulder position with the shoulder circumference) (B). dNo relationship between AHD and age, height, weight, and arm length was found except individuals with narrower AHD in the rest neutral position had smaller shoulder circumferences (r = 0.42, p = 0.04). Individuals with longer years of injury had a greater AHD percentage decrease after WR (r = -0.55, p = 0.01). Subjects with a larger AHD in the unloaded neutral position have greater AHD decreases in the weight relief loaded position (r = -0.58, p < 0.01). A higher shoulder pain score on WUSPI was associated with a smaller AHD after shoulder external rotation exercise (r= -0.45, p = 0.03). Stepwise linear regression found shoulder circumference is a predictor of AHD in the shoulder neutral position (β= 0.42, p = 0.04) and years since injury is a predictor of AHD decreases after WR (β= -0.58, p < 0.01) (Figure 2).
DISCUSSION
This study is the first to investigate the relationship between ultrasonographic-measured subacromial space and muscle fatigue in a population who is highly prone to shoulder problems. The AHD decreased in subjects who had confirmed EMG signs of muscle fatigue after WR and ER. This finding is in agreement Chopp et al. (Chopp, et al., 2010) who found healthy participants showed superior migration of humeral head after fatigue. Teyhen et al. (Teyhen, et al., 2008) also found that individuals without shoulder disorders demonstrated superior migration of humeral head during arm elevation after fatiguing the rotator cuff muscles. These other studies examined AHD during shoulder elevation. With elevation, the deltoid enhances the upward pull of the humerus. This would likely magnify the upward shift of the humeral head in the arm elevation position compared to the weight relief position in which the deltoid muscle does not play as significant of a role (Reyes, Gronley, Newsam, Mulroy, & Perry, 1995) . We chose this position because it provides a functional measure of what the AHD looks like under realistic loading conditions. Not finding greater differences in the AHD measures could mean that compensatory muscles or strategies enabled the space to be preserved post-fatigue of the external rotators in this position. We found participants with narrower space after shoulder external rotation exercise has larger pain score. The finding is valuable because shoulder external rotation is frequently recommended during isotonic rotator cuff strengthening exercises for individuals with subacromial impingement syndrome. The narrowing AHD applied compression overstressed on the supraspinatus tendon to diminish the flood flow (Fu, Harner, & Klein, 1991). Future studies are needed to investigate various shoulder positioning effects in both loaded and unloaded states on the AHD measure.
Shoulder neutral position was related to shoulder circumference and suggests that future studies should consider normalizing the AHD or statistically controlling for this anatomical measurement. The positive correlation between years of injury and AHD percent decreases held true after controlling for shoulder circumference. Our results point to the potential harmful effects of repeated weight-bearing activities and overuse on the space. Thus interventions that target preservation of the subacromial space are critical for wheelchair users due to their long life expectancies. Finding differences for weight-relief raises in the AHD warranty additional studies to investigate acute AHD changes after other weight-bearing activities such as intense wheelchair propulsion. If the AHD change relates to biomechanical indicators such as force and cadence, interventions to preserve the space may include propulsion training or a lighter weight wheelchair. This study could provide more insight into the mechanisms leading to subacromial impingement syndrome.
CONCLUSIONS
Subacromial space assessment using ultrasound provided reliable measures and detected AHD narrowing after global and local muscle fatiguing tasks. Individuals who experienced longer years since injury were most likely to exhibit greater decreases in the AHD after multiple weight relief push-ups. AHD in the unloaded position was related to shoulder circumference and percentage changes in the AHD and AHD narrowing after ER was associated with shoulder pain. Future studies of AHD considering shoulder anatomical normalization are warranted. Biomechanical variables such as joint forces and positioning during weight-bearing activities may help identify causes of subacromial space reduction and help guide clinical interventions such as wheelchair training or wheelchair prescription to preserve upper extremity function among wheelchair users.
REFERENCES
ACKNOWLEDGEMENTS
This material is based upon work supported by the Department of Veterans Affairs Rehabilitation Research and Development Service (Project Number: B6789C) and the Paralyzed Veterans of America. This material is the result of work supported with resources and the use of facilities at the Human Engineering Research Laboratories, VA Pittsburgh Healthcare System. The contents of this abstract do not represent the views of the Department of Veterans Affairs or the United States Government.