Phillip M. Grice, Yash Chitalia, Megan Rich, Henry M. Clever, Charles C. Kemp
Healthcare Robotics Laboratory, Georgia Institute of Technology, GA, USA.
ABSTRACT
Individuals with severe motor impairments often have difficulty operating the standard controls of electric beds and so require a caregiver to adjust their position for utility, comfort, or to prevent pressure ulcers. Assistive human-computer interaction devices allow many such individuals to operate a computer and web browser. Here, we present the Autobed, a Wi-Fi-connected device that enables control of an Invacare Full-Electric Homecare Bed, a Medicare-approved device in the US, from any modern web browser, without modification of existing hardware. We detail the design and operation of the Autobed. We also examine its usage by one individual with severe motor impairments and his primary caregiver in their own home, including usage logs from a period of 102 days and detailed questionnaires. Finally, we make the entire system, including hardware design and components, software, and build instructions, available under permissive open-source licenses.
INTRODUCTION


Our results suggest that this module enhances the independence of individuals with severe motor impairments by enabling them to control their bed without the assistance of a caregiver. It also appears to facilitate the caregiver’s work as it requires little effort for sustained operation, and reduces the need to adjust the patient’s bed. By using a web-based interface, the Autobed avoids the cost or obstruction of a dedicated assistive input, instead relying on whatever human-computer interaction (HCI) technology the user already employs.
The idea for Autobed was originally presented by Mr. Henry Evans during our work together. Henry has quadriplegia and is mute as the result of a brain-stem stroke, and has only limited movement in his head and left arm and hand, although he has full sensation. Henry regularly uses a computer via a head-tracking mouse from NaturalPoint, Inc. Henry and his wife and primary caregiver Jane have used and tested multiple versions of the Autobed continuously in their own home, and feedback from both has guided the user-centered design process we employed with the Autobed.
RELATED WORK
Environmental control units (ECUs) have been deployed in hospital and domestic settings for over half a century (Dickey & Shealey, 1987). However, ECU’s often include specialized hardware for user input, raising the cost of the unit. Instead, the Autobed system allows those already using an assistive HCI device to multiplex the HCI’s interface for also controlling the bed (Fig. 1, left).
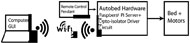
Recently, a large number of everyday devices are being equipped with wireless transmitters/ receivers, allowing them to connect to the internet, and establishing the category of “Internet of Things” (IoT) (Mattern, 2010). Here, we demonstrate one approach to converting a standard domestic electric bed into an IoT device.
SYSTEM DESCRIPTION
| Actuator | Up | Down |
|---|---|---|
Head |
25s | 24s |
Bed |
25s | 21s |
Feet |
10s | 10s |
In the standard Invacare bed, a separate motor drives each of the Invacare Full Electric hospital bed’s three movements, and each can be run forward or backward to drive the attached mechanism as desired. All three motors are controlled from a single motor control board, to which a wired remote pendant connects. Six momentary switch buttons on this remote each complete low-voltage, low-current circuits, which activate mechanical relays on the motor control board, in turn activating the associated motors. By electrically completing these control circuits, and so mimicking the effects of the remote pendant’s physical switch, we are able to electronically activate each motor and control the bed.
The Autobed consists primarily of a small, low-power Raspberry Pi computer. This computer connects to the user’s home Wi-Fi network, and serves an HTML-based GUI with six large, responsive buttons (see Figure 2) to any devices on the local network via an Apache 2.0 web server. This interface then sends commands via a websocket connection back to a Python Tornado-based server on the Raspberry Pi. This server then uses the 3.3V General-Purpose Input/Output (GPIO) pins on the Raspberry Pi to activate one of six optoisolators which complete the bed’s control circuits and drive the motor relays, mimicking the pendant buttons. These optoisolator circuits are connected in parallel to the handheld remote pendant, which continues to operate normally through the Autobed, even when the Autobed module is not powered (Fig. 3).
The web interface sends a command every 75ms while a GUI button is depressed. Upon receiving a command, the Raspberry Pi server drives the indicated function for 155ms. This allows for smooth motion even if commands are delayed, but keeps the interaction on the order of 0.1 seconds, in which range users typically perceive interactions as fluent. This timing also provides accurate control of the bed, as each 155ms active period moves the head angle and bed height <1% of their total travels, and moves the legs of the bed only ~1.5% of its total travel (see Table 1).
The Autobed connects in-line with the remote control pendant, so it is not necessary to modify the bed hardware. However, the Invacare Owner’s Manual indicates that owners should “use only authorized Invacare replacement parts and/or accessories otherwise the warranty is void” (Invacare, 2007).
The Raspberry Pi and optoisolator circuit are housed in a plastic enclosure, providing mechanical protection for the system. The enclosure exposes a female RJ45 socket to attach the standard control pendant, a male RJ45 cable which connects to the motor control board socket in place of the hand pendant, and a power cord.
RESULTS
We installed an initial version of the Autobed in the Evans’ home on June 24th, 2014, and installed a second version, with an interface similar to that described above, on October 14th, 2014. We installed the version, detailed here, on October 12th, 2015. Complete design details, with build instructions and links to all software, can be found at (Grice, 2016).
Data Collection
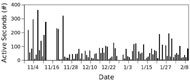
At the end of the 102 days we asked Henry and Jane Evans each to complete a questionnaire composed of both Likert items and open-ended questions. Questions related to their adoption and use of the Autobed, and were based on the Technology Acceptance Model (Davis, 1989), in particular asking about factors contributing to Perceived Usefulness and Perceived Ease of Use, based on (Chen, 2014) and (Davis, 1989). In addition, we also asked for their insights into recorded usage trends, and how they believed the Autobed impacted their lives, as well as any challenges or opportunities for improvement.
Usage Statistics
We also examined the distribution of function use between the three controls on the bed based on number of active seconds in the full trial period. Most (91.7%) of use involved adjusting the head of the bed. After that, most of the remaining use (7.5%) involved adjusting the legs, and only 0.5% of the active seconds involved adjusting the bed height. Both Henry and Jane also ‘strongly agreed’ that these data are correct.
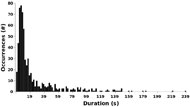
We also examined the duration of sessions of interaction between the user and the Autobed. We define a session as a series of commands which may be separated by periods of inactivity less than 1 minute.
The median session duration is 10s, though the shortest lasted only 1 second, and the longest lasted 238s (3 minutes 58 seconds) (Fig. 6).
Henry Evans, “agreed” or “strongly agreed” with all six Likert items regarding Perceived Usefulness, and “slightly agreed” or “agreed” with all items regarding Perceived Ease of Use. Both Henry and Jane “strongly agreed” that Henry uses the Autobed often, that it is reliable, and that it makes Henry more independent.
DISCUSSION
Pressure Ulcer Prevention
The generally accepted solution to prevent pressure ulcers is to turn the patient once every two hours (Ostadabbas et al., 2011). However, this may be difficult to achieve, especially for family caregivers with other duties. The Autobed allows patients to take some measures for themselves to relieve pressure, and is especially useful for individuals such as Henry who retain sensation and can recognize pressure build-up. While Henry did not respond to this item, Jane “strongly agreed” that the Autobed helps Henry maintain and improve his health. Both Henry and Jane indicated that the Autobed helps Henry relieve pressure build-up.
Caregiver Perspective
Despite prior research highlighting the importance of designing assistive technologies to be usable for caregivers (Kintsch, et al., 2002), Henry still finds that this is a limitation of many assistive technologies. Henry regularly emphasizes the importance of assistive technologies both being easy for caregivers to use and making the caregiver’s life easier (Evans, 2016). Our results suggest that the Autobed meets this requirement. Jane “strongly agreed” with all items relating to Perceived Usefulness of the Autobed as a caregiver, except she “disagreed” that the Autobed improves her performance in caregiving, stating that “it has nothing to do with attitude or capability.” She “strongly agreed’ that the Autobed is easy to use, and easy to learn to use as a caregiver, but “disagreed” that it was easy to control and that her interaction was clear and understandable, stating that “[she has] never tried it” and “[she doesn’t] interact at all with the Autobed except if a wire becomes loose,” both of which indicate that the Autobed requires little attention from a caregiver, and emphasizes that Henry is the user.
CONCLUSION
The Autobed represents an open-source method of enabling web control of a commercially available hospital bed to assist individuals with severe motor impairments. By using a web-based interface, a user with motor impairments does not need a dedicated interface such as for an ECU, and can effectively manage his own comfort. We show that the device is reliable, and requires little interaction from caregivers, enhancing the likelihood of adoption, while granting the motor-impaired user increased independence.BIBLIOGRAPHY
Basmajian, A., Blanco, E. E., Asada, H. H., & IEEE. (2002). The marionette bed: Automated rolling and repositioning of bedridden patients. Robotics and Automation, 2002. ConferenceProceedings. ICRA’02. IEEE International Conference on, 2, pp. 1422-1427.
Chen, T. L. (2014). Haptic interaction between naive participants and mobile manipulators in the context of healthcare. Dissertation.
Davis, F. D. (1989). Perceived usefulness, perceived ease of use, and user acceptance of information technology. MIS quarterly, 319-340.
Dickey, R., & Shealey, S. H. (1987). Using technology to control the environment. American Journal of Occupational Therapy , 41 (11), 717-721.
Evans, H. (2016). Evaluating Assistive Devices. Retrieved from https://www.youtube.com/ watch? v=LCvp1Ioh9pA. Cal-Tech MedE105. Guest Lecture.
Ostadabbas, S., Yousefi, R., Nourani, M., Faezipour, M., Tamil, L., Pompeo, M., et al. (2011). A posture scheduling algorithm using constrained shortest path to prevent pressure ulcers. Bioinformatics and Biomedicine (BIBM), 2011 IEEE International Conference on, (pp. 327-332).
Gillespie, B. M., Chaboyer, W. P., McInnes, E., Kent, B., Whitty, J. A., & Thalib, L. (2014). Repositioning for pressure ulcer prevention in adults. Cochrane Database of Systematic Reviews (4).
Grice, P. M., Chitalia, Y., Rich, M., Clever, H., Evans, H., Evans, J., & Kemp, C. C. (2016, February 3). Autobed: A Web-Controlled Robotic Bed. Retrieved from http://www.webcitation.org/6f1U8gndP
Invacare, Inc. (2007, August). Owner’s Operator and Maintenance Manual: IVC Bed Series [Rev. F]. Ohio, Elyria.
Kintsch, A., & DePaula, R. (2002). A framework for the adoption of assistive technology. SWAAAC 2002: Supporting learning through assistive technology, 1-10.
Mattern, F., & Floerkemeier, C. (2010). From the Internet of Computers to the Internet of Things. Springer.
Seo, K.-H., Oh, C., Choi, T.-Y., & Lee, J.-J. (2005). Bed-type Robotic System for Bedridden.
Van Der Loos, H. M., Ullrich, N., & Kobayashi, H. (2003). Development of sensate and robotic bed technologies for vital signs monitoring and sleep quality improvement. Autonomous Robots , 15 (1), 67-79.