MacIntosh A.1-5, Vignais N.1, Vigneron V.2, Fay L.3,5, Musielak A4, Desailly E.4, Biddiss E.3,5
1Université Paris-Saclay, Univ. Paris-Sud et Univ. d'Orléans CIAMS, France, 2Université Paris-Saclay, Univ. Evry, IBISC, France, 3Bloorview Research Institute, Canada. 4Fondation Ellen Poidatz, France, 5University of Toronto, IBBME, Canada.
INTRODUCTION
Cerebral palsy (CP) is a disability due to brain injury or abnormality near birth and persists through the lifespan [1] . CP can impact a person’s motor control, perception, intellectual function, ability to perform daily activities and participation in society [2] . Persons with CP can have impaired hand or arm function affecting motor activities.
Interventions that improve motor activities often require frequent and intense practice . The feedback a person receives during practice is also critical. Feedback impacts how readily someone learns a task, their focus, and motivation [4] . Biofeedback, where information about a motor performance is given back to the individual, can help increase awareness and control that normally goes unnoticed [5] . However, a recent review of interventions using biofeedback for people with CP found that ineffective biofeedback strategies were commonly employed [3] . Traditionally, biofeedback has been given in a way that may slow development. It forces the person into a passive role in their practice and builds dependence on the feedback [6] .
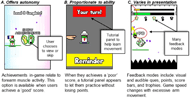
Biofeedback strategies should reflect current clinical evidence and motor learning theory. An evidence-based biofeedback strategy: a) offers autonomy, making people active contributors to their practice and builds a sense of ownership b) is proportionate to the person’s ability, and c) varies in presentation. These biofeedback principles can enhance motivation, independence and self-efficacy [3,7] .
In this project, we have built an active video game using these biofeedback principles. The technology serves to improve the efficacy of home-based exercise for young people with CP. We hypothesize that embedding evidence-based biofeedback into new technology will help participants actively engage with their habilitation. Specifically, the study aims for participants to:
- choose to review their performance when presented the opportunity
- adapt their movements immediately after being given biofeedback
- improve their performance as the task becomes more difficult
METHODS
Developing the active video game technology
We consulted young people with CP and clinicians to build a new active video game technology. Users control a character on-screen by making therapeutic hand gestures. We worked with an independent game developer (KasSanity Inc.) to modify a commercial game. The modified game supported the adapted controller and incorporated biofeedback principles. Development occurred through semi-structured interviews and game testing sessions between June 2017-May 2018. Raw data from the Myo Armband (Thalmic Labs, Kitchener, Ca) (eight-channel electromyography (EMG) and 9-axis inertial measurement unit (IMU)) were processed through custom software (MATLAB 2017b) to interpret gestures that commanded the game. Details of the construction of the game controller are presented elsewhere [8].
Stakeholders iteratively contributed to design the biofeedback presentation and timing during the game testing sessions. Key biofeedback principles were implemented as outlined in Figure 1. After designing the new active video game technology, we evaluated how young people with CP responded to evidence-based biofeedback while practicing alone in a home-based intervention.
Using the active video game technology in a home-based intervention
Before playing the game at home, participants completed assessments of hand strength and mobility five times. They also created a self-defined practice schedule with the assistance of their caregiver and the therapist (the suggested goal was 3-5 times per week, 30 minutes per day). Then each participant took home a laptop and Myo Armband to play for four weeks. Once per week, the researcher visited the participants to assess hand strength and mobility. The researcher also evaluated the participants motivation and adherence to the self-defined practice schedule through semi-structured interview. Outcomes related to functional changes and intervention feasibility are being presented in a separate manuscript. The system automatically collected biofeedback usage data. Participant observations related to biofeedback were also recorded during the weekly semi-structured interview.
Analysis
Aim 1, review performance. The proportion of opportunities participants took to view their achievements was used to evaluate the extent to which participants actively engaged with their exercise. How frequently participants decided to review their performance as opposed to directly playing the next level is an indication of their interest in improving the activity and their engagement with the exercise.
Aim 2, adapt after biofeedback. Immediate, in-level changes in performance were measured by the change in arm movement (resultant angular velocity) before and after showing a ‘speed-change biofeedback event’. The percent change in arm movement five seconds before compared to five seconds after the biofeedback event shows to what extent participants adapted after feedback.
Aim 3, improve performance from biofeedback. The change in how often participants required a tutorial panel showes longer-term variations in performance. Seeing a tutorial panel alerts the participant to a poorly timed or executed movement. So as game difficulty increases, a player who is improving would see fewer tutorial panels, while a player who is not improving would see as many or more tutorial panels over time.
To complement these metrics, participants answered questions about how they played and what motivated them. Examples prompts include: “How fair, do you feel, was your score in the game?” and “Did you find the game was too easy/ too difficult?” [10] . Demographic characteristics and system usage are presented descriptively to provide context. Wilcoxon signed ranked tests were used to evaluate the change in biofeedback usage between the first half (weeks 1-2) and the second half (weeks 3-4) of the intervention. Alpha was set to 0.05 and Hodge-Lehmann confidence intervals are presented [11]. All reported metrics are mean ± standard deviation across participants.
RESULTS
There were four female and five male participants 11.6±2.8 years old. Four were at MACS level II and five at level I. Six had mixed tone and three had spastic hemiplegia. During the four-week intervention participants averaged 161±64 wrist extension gestures each day played. They played an average of 15±5 minutes per day, 4±1 days/per week. Of that time, 53% was actively practicing (in-level).
Aim 1, review performance. Participants chose to view their achievements 62.1±15.9% of the time. This stayed consistent across the intervention with participants choosing to view achievements 71.5±23.8% in the first half of the intervention and 57.0±18.6% in the second half (p=0.3, 95%CI=-37-12%, view percent change). To this point, 6/9 participants remarked that they decided to review their achievements as they aimed to get all the trophies in each level.
Aim 2, adapt after biofeedback. Participants completed wrist extension gestures with better isolation directly after biofeedback. After the ‘speed-change biofeedback event’, the variability of forearm resultant angular velocity decreased by 12±4% (p=0.004, 95%CI=-16 - -9%).This response to biofeedback was consistent across the intervention (an 11±3% decrease in the first half and a 13±5% decrease in the second half, p=0.16, 95%CI=-5-1%).
Aim 3, improve performance from biofeedback. Each time a tutorial panel is shown it lets the participant improve their performance before continuing the level. Participants required tutorial panels less frequently as difficulty increased. In level 1, 1.8±0.7 tutorial panels were shown compared to level 10, where 0.8±0.3 panels were shown (p=0.03, 95%CI=-1.6--0.2, change in panels/level). Accordingly, participants commented that the game provided them with the ‘right amount of challenge’. Tutorial panels were presented at a similar frequency across the intervention. (1.8±0.8 panels/level in the first half compared to 1.4±0.6 in the second half, p=0.07, 95%CI=-1- 0.2 panels/level).
DISCUSSION
This study shows how young people with CP can engage with and respond to biofeedback in a home-based intervention. Participants:
- often choose to review their performance,
- can respond immediately to biofeedback while practicing at home,
- use biofeedback to improve their longer-term performance.
The biofeedback was multi-modal and addressed different aspects of the motor activity. Participants received biofeedback when they achieved high forearm extensor activity while keeping flexor activity low (co-contraction). Biofeedback was also related to the ability to isolate hand movement. These motor aspects had different presentations. Varying presentation, changing when feedback is received and what it looks like, can help individuals avoid dependence on the feedback itself [7,12] . Immediate in-level feedback contributed to overall performance which participants reviewed at the end of the level. This approach gave participants a general impression of their ability and motivated them towards higher quality movements.
Participants took advantage of the autonomy offered through this biofeedback intervention. Game scores related to quality of forearm co-contraction. So, in choosing to view performance participants could develop an inherent sense of their muscle activity while playing. This type of autonomy has been found to build investment in an activity [4] . Participants wanted trophies and to unlock characters. Their comments reflect the importance of linking game rewards to therapy goals. Similarly, requiring fewer tutorial panels as difficulty increased shows players developed competency in the motor activity. Providing a fading feedback schedule and only offering biofeedback when players are in a ‘target zone’ can lead to improvements in performance and retention [6] . Based on participant’s performance and comments, the semi-automated tailoring of biofeedback here seems an appropriate step towards helping young people with CP build self-reliance in motor activities at home.
Adapting an existing game with commercial success was advantageous. It offered quick content to test with participants, leaving more time to focus on biofeedback. However, considerable time was invested working with the company appropriately integrate the biofeedback. Teams should consider adapting professional games, especially when artistic and developer resources are limited. To facilitate the use of evidence-based biofeedback, an infographic has been developed. The infographic, at the Holland Bloorview PEARL lab website, is targeted for multi-disciplinary teams looking to build programs the help people improve motor activities.
Study results suggest that biofeedback was delivered reasonably well, however where was considerable in-level feedback during the last weeks of practice. This could have slowed participants from exploring new movement strategies. Further, participants used self-directed practice schedules to maximize ownership and motivation at home. Certain participants played infrequently some weeks (e.g. due to school assignments or competing interests). Finally, game difficulty (e.g. speed, obstacle frequency) adjustments were based on general proficiency in the movement and the game as observed by the researcher because of inconsistent and varying practice schedules. These limitations will be considered for future iterations of the technology.
CONCLUSION
A new home-based therapy activity was developed for young people with CP. It was built from the ground up using evidence-based biofeedback strategies. This study shows that participants can positively engage with biofeedback in home-based activities towards improving motor outcomes. Participants took autonomy over reviewing their performance and adapted in the short and long term in response to biofeedback. We will continue to evaluate the effect of these biofeedback strategies in the second phase of data collection. The strategies used in this study can be applied to other technologies to maximize the health and well-being of people with neuromotor disorders. To aid in this knowledge transfer, an infographic is available highlighting important considerations when using biofeedback.
REFERENCES
[1] Rosenbaum P, Paneth N, Leviton A, Goldstein M, Bax M, Damiano D, et al. A report: The definition and classification of cerebral palsy April 2006. 2007 Feb;49(SUPPL.109):8–14.
[2] Novak I, Mcintyre S, Morgan C, Campbell L, Dark L, Morton N, et al. A systematic review of interventions for children with cerebral palsy: State of the evidence. 2013;55(10):885–910.
[3] Macintosh A, Lam E, Vigneron V, Vignais N, Biddiss E, Lam, et al. Biofeedback interventions for individuals with cerebral palsy: a systematic review. 2018 May 12;1–23.
[4] Wulf G, Shea C, Lewthwaite R. Motor skill learning and performance: a review of influential factors. 2010 Jan;44(1):75–84.
[5] Van Dijk H, Jannink MJ a, Hermens HJ, Van Dijk H. Effect of augmented feedback on motor function of the affected upper extremity in rehabilitation patients: a systematic review of randomized controlled trials. 2005 Jul 1;37(4):202–11.
[6] Timmermans AA, Seelen HA, Willmann RD, Kingma H, Truelsen T, Piechowski-Jozwiak B, et al. Technology-assisted training of arm-hand skills in stroke: concepts on reacquisition of motor control and therapist guidelines for rehabilitation technology design. 2009;6(1):1.
[7] Wulf G. Self-controlled practice enhances motor learning: implications for physiotherapy. 2007;93:96–101.
[8] MacIntosh A, Vignais N, Biddiss E, Vigneron V. Reach and grasp motion recognition for virtual rehabilitation of youth with cerebral palsy. In Dublin, Ireland; 2018.
[9] Eliasson AC, Krumlinde-Sundholm L, Rösblad B, Beckung E, Arner M, Öhrvall AM, et al. The Manual Ability Classification System (MACS) for children with cerebral palsy: Scale development and evidence of validity and reliability [Internet]. Cambridge University Press; 2006. p. 549–54.
[10] Ni L, Fehlings D, Biddiss E. Design and Evaluation of Virtual Reality-Based Therapy Games with Dual Focus on Therapeutic Relevance and User Experience for Children with Cerebral Palsy. 2014;3(3):162–71.
[11] Lehmann EL, D’Abrera J. Nonparametrics: Statistical Methods Based on Ranks. 2006;1–5.
[12] Sigrist R, Rauter G, Riener R, Wolf P. Augmented visual, auditory, haptic, and multimodal feedback in motor learning: A review. 2013;20(1):21–53.Acknowledgement
This work was supported by the Canadian Institute of Health Research (RN304779—379428), Mitacs GlobaLink, and Campus France. The authors are grateful to the Univ Evry, Université Paris-Saclay IT department head, Remy Boyer, and to Ajmal Khan at the Bloorview Research Institute for their technical support in making this data collection possible. Finally, our greatest appreciation goes to the families who volunteered their time to this project, without whom we would have neither impetus nor ability.