Assessment of Gait and Outcome Measures in Children with Type I Osteogenesis Imperfecta
*Graf, A, *Hassani, S, *Smith, P, +Caudill, A, +Flanagan, A, *+Harris, G.
*Shriners Hospitals for Children, Chicago, IL
+Orthopaedic & Rehabilitation Engineering Center (OREC) Marquette University/Medical College of Wisconsin, Milwaukee, WI
ABSTRACT/BACKGROUND:
It is estimated over 50,000 people in the U.S. have Osteogenesis Imperfecta (OI), also known as “brittle bone disorder.” OI is a genetic disorder causing a defect in collagen synthesis and can produce a broad variability of expression including skeletal fractures, bone fragility, ligamentous laxity and muscle weakness, short stature, hearing loss, scoliosis, skull and long bone deformities, blue sclerae, deafness, and teeth abnormalities1. There is no cure for OI but bisphosphonate medical treatment and surgery are used for disease management. Treatment of OI includes managing/preventing fractures and maximizing function. There are several forms of OI, representing a wide variation in appearance and severity. Type I OI is the mildest type and most common. They are community ambulators of normal or slightly reduced stature but are susceptible to frequent bone fractures, loose joints and muscle weakness, and spinal curvature. This study evaluated gait parameters and outcome measures (Pediatric Outcome Data Collection Instrument (PODCI), Gillette Functional Assessment Questionnaire (FAQ), Faces Pain Scale-Revised (FPS-R)) in children with Type I OI as part of a broader investigation to understand and predict bone fracture through biomechanical modeling of the lower extremities. Gait characteristics and outcome assessments of children with mild OI have not been reported. In this study, gait characteristics and outcome measures in children with Type I OI were compared with age-matched controls. Ultimately, we hope to offer an improved treatment approach and a better quality of life to children with mild OI by using gait analysis and outcome assessment tools.
KEY WORDS:
Osteogenesis Imperfecta (OI), kinematics, outcome assessment, brittle bone disorder
METHODOLOGY:
Ten Type I OI subjects (6 M, 4 F; 12.4 ± 3.5 years of age) and twenty-two controls (14 M, 9 F; 10.3 ± 3.1 years of age) participated in this IRB-approved protocol. All OI subjects completed the baseline Pediatric Outcome Data Collection Instrument (PODCI) and the Faces Pain Scale-Revised (FPS-R). The OI participants were all good community ambulators without assistive devices, as evidenced by scoring a minimum of 9 out of 10 in the Gillette Functional Assessment Questionnaire (FAQ). Kinematic data of the lower extremities was measured using a 14-MX camera three-dimensional motion analysis system (VICON, Motion Analysis Corp., Santa Rosa, CA, USA). Two force-plates (AMTI, Newton, MA) embedded in the walkway were used to collect kinetic data. Comparisons between the two groups were made by using unpaired nonparametric methods, Wilcoxon- Mann-Whitney test (significance at p<0.05). Within the OI group, left and right side temporal spatial parameters, kinematics and kinetics were not significantly different at the hip, knee, and ankle.
RESULTS:
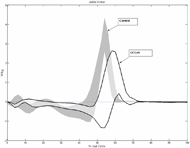
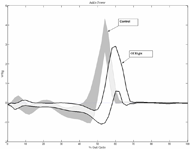
All ten OI patients indicated a FPS-R score of zero (no pain) during the time of their testing. As shown in Table I, walking speed (meters/second) and toe off (% gait cycle) were significantly lower in the OI group when compared to the controls. Kinematics at the hip, knee and ankle revealed a few significant differences from normal for this sample size with diminished mean maximum plantarflexion during third rocker for the OI group (left OI:-7.5 º ± 10.2 º; right OI: -7.8º ± 10.3º; and controls: -11º ± 6.4º). Ankle push off power was also significantly reduced and delayed in the OI group when compared to the controls (left OI: 2.5± 0.6 W/kg at 58% gait cycle; right OI: 2.7 ± 0.5 W/kg at 57% of the gait cycle; and controls: 3.6 ± 0.5 W/kg at 52 % of the gait cycle) (Graphs I and II).
|
Walking Speed (m/s) |
Toe Off (%GC) |
||
|---|---|---|---|---|
|
Left |
Right |
Left |
Right |
| OI Subjects | 1.04(0.1)* |
1.05(0.1)* |
63.52(2.3)* |
63.34(2.4)* |
| Controls | 1.17(0.1) |
1.16(0.1) |
60.26(1.7) |
61.08(1.2) |
| * P value ≤ 0.05 | ||||
| Sub-Category | Mean (SD) |
Max Score |
Upper Extremity & Physical Function |
94.8 (8.4) |
100 |
|---|---|---|
Transfers & Basic Mobility |
98.0 (3.7) |
100 |
Sports & Physical Function |
76.9 (17.9) |
100 |
Pain/Comfort |
85.6 (14.1) |
100 |
Happiness |
80.5 (17.4) |
100 |
Global Function & Symptoms |
88.9 (7.0) |
100 |
Expectations |
68.4 (26.1) |
100 |
Subscales of the PODCI were evaluated with maximum sub-score of 100 (Table II). The OI patients had high average sub-scores in the areas of Upper Extremity and Physical Function (94.8 ± 3.6), Transfers and Basic Mobility (98.0 ± 6.7), and Global Function and Symptoms (88.9 ± 7.0). They had lower average sub-scores in the areas of Sports and Physical Function (76.9 ± 17.9) and Expectations (68.4 ± 26.1). Of the OI patients, six scored the highest score of ten on the FAQ, but four had scores of nine, indicating they are good community ambulators, but may experience difficulty or require minimal assistance with running, climbing, and/or stairs. They also may experience difficulty keeping up with peers.
DISCUSSION:
Clinical features of children with Type I OI can vary widely. In our pilot study, subjects did not complain of pain but, exhibited a deficiency in gait indicated by their slower walking speed, kinematics and kinetics. With an increased stance phase and diminished ankle motion, the OI patients are generating a reduced ankle push off power. This is most likely from subtle weakness, ligamentous laxity, and avoidance of excessive forces which may cause injury. These findings are consistent with their outcome assessments scores (PODCI and FAQ) where they exhibit limited sports and physical function and may experience difficulty running and climbing stairs. Their physical activity limitations further contribute to muscle and bone weakness. Understanding the clinical manifestations seen in children with Type I OI may help the clinician provide better medical care and an improved quality of life for patients with OI. Better rehabilitation programs are needed to improve muscle strength and increase their physical activity while reducing fracture risk. Gait analysis and outcome assessment can be used to assess affects of treatment.
REFERENCES:
- Long J, Rhode H, Smith P, Harris G. (2000): Osteogenesis Imperfecta: Physiology, Manifestations, Mobility, and Treatment, In Pediatric Gait: A New Millennium in Clinical Care and Motion Analysis Technology, 1st edition, Harris, G., and Smith, P., Eds., IEEE Press, New York, C-17, 124-133.
- Sillence DO, Senn A, Danks DM. (1979) Genetic heterogeneity in osteogenesis imperfecta. J. Med. Genet. 16, 101-116.
ACKNOWLEDGEMENTS:
Supported by funds from OREC, Shriners Hospitals for Children, and NIDRR Grant H133P02004
AUTHOR CONTACT INFORMATION:
Adam Graf
Shriners Hospitals for Children – Chicago
Motion Analysis Laboratory
2211 N. Oak Park Ave.
Chicago, IL 60707
(773)385-5458
agraf@shrinenet.org
Highlights
- Source Ordered
- No Tables
- Very Compatible
Gargoyles
Disney produced a television show in the mid 1990s called Gargoyles. It's a great show and I'm a big fan. A few years ago Disney started to release the show on DVD. The last release was of season 2, volume 1. That was two years ago. Volume 2 has not been released. Why? Poor sales. So if you should find yourself wanting to support my work, instead I ask you pick up a copy of season 2, volume 1. It's a great show and you might find yourself enjoying it.